New modeling shows that 'shielding' strategies instead of lockdowns would have led to tens of thousands more deaths

Shielding those vulnerable to COVID-19, while allowing the virus to spread, largely unmitigated, through the rest of the population, would have failed according to a new modeling paper published today in PLOS Global Public Health by University of Bath scientists.
Shielding strategies or "focused protection", as advocated for in the Great Barrington Declaration, would have been impossible to implement in practice and would have likely led to far worse outcomes. Even if implemented perfectly, the modeling reveals that allowing the infection to spread through less vulnerable groups prior to vaccination would have overwhelmed health care capacity in the UK and led to tens of thousands of unnecessary deaths. In reality, practical considerations would have meant that large numbers of vulnerable people who were supposed to be protected would also have died.
The unprecedented scale of the public health crisis posed by the COVID-19 pandemic forced governments around the world to impose restrictions on social contact to suppress transmission of the coronavirus. However, the social and economic costs of these measures, especially lockdowns, have been high, drawing substantial opposition from some sections of the media, members of the public, and a small, but vocal group of scientists.
An alternative and widely discussed strategy would have been to temporarily focus protection on ("shield") those who were most vulnerable to COVID-19 (the elderly and those with certain pre-existing conditions), with the aim of achieving herd immunity by allowing a largely unmitigated epidemic in the rest of the population. However, this approach has received little scrutiny in the form of mathematical modeling.
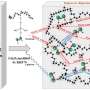
In this new study, published today, the researchers assessed a hypothetical large city in England with a population of 1 million inhabitants, using an SEIR (Susceptible, Exposed, Infected, Removed) model. They compared the outcomes from no shielding, with imperfect and perfect shielding, with shielding restrictions lifted when cases fall below a given threshold.
The research concludes that while shielding may have protected the vulnerable in theory, it required extremely restrictive conditions that were impossible to achieve in practice. For example, because shielding in real populations would have been imperfect, infections in the lower-risk population would have leaked through to vulnerable people who were shielding. In addition, if lower-risk individuals reduced social contact to avoid infection it may have been impossible to achieve herd immunity, meaning a second wave of infections would have occurred after shielding had ended. Even if herd immunity was achieved, care homes would still have been at risk of local outbreaks because immunity would have been unevenly distributed in the population.
To be effective, shielding would have required those who were at higher risk to not only be rapidly and accurately identified, but also to shield themselves for an indefinite period, rendering the strategy impractical to implement. The modeling also suggests that in even the most optimistic shielding scenario, critical care capacity in hospitals would have been exceeded at least ten-fold at the peak of the outbreak. This is not to mention the huge healthcare burden associated with the large number of cases of long COVID that would result from mass infection. Waning immunity, and new immunity-evading variants would only have served to make a shielding-only strategy even more untenable.
Although vaccines are now available and have been successfully rolled out in many countries, modeling studies such as this are critical to determine whether shielding would have been a viable strategy for dealing with COVID-19, or, indeed, the next pandemic. Many countries have poor vaccine coverage and so the choice between shielding and measures that are more restrictive at a population level is likely to remain for some time. In future, new variants may continue to emerge that are able to escape immunity, which may require a renewed choice between lockdowns and shielding.
In summary, the new study exposes critical weaknesses of shielding (or focused protection): even with the most optimistic assumptions, tens of thousands of lower-risk individuals would have died and critical care capacity would have been rapidly exceeded. With more realistic assumptions, shielding would have failed to protect the most vulnerable, achieving little more protection than an unmitigated epidemic.
Dr. Kit Yates, senior lecturer in the Department of Mathematical Sciences at the University of Bath and one of the study's authors, explains: "Our study shows how misguided the idea of shielding the vulnerable and letting the virus rip through the rest of the population would have been.
"Even if we could have managed perfect shielding, our healthcare system would still have been quickly overwhelmed. In reality, some inevitable leakiness in the shielding system would almost certainly have led to big outbreaks amongst the vulnerable and resulted in huge numbers of deaths as well."
Dr. Cameron Smith, another of the study's authors, added: "Our model captures some important features which represent how immunity is likely to be distributed in the population. As a consequence of this heterogeneity, potential shielding strategies would have had limited success in reducing the number of deaths."
Dr. Ben Ashby, the study's other author said: "Despite the success of the vaccination program, the recent omicron wave shows that we are not out of the woods yet. If in future a new variant emerges that substantially escapes existing immunity, then it's possible we may have to choose between lockdowns and shielding once again (or indeed, in future pandemics). Although lockdowns are costly for many reasons, attempting to shield the vulnerable while letting the virus spread through the rest of the population is far worse."
More information: Critical weaknesses in shielding strategies for COVID-19, PLOS Global Public Health (2022). DOI: 10.1371/journal.pgph.0000298