Magnetic therapy enhances chemotherapy treatment of breast cancer
Breast cancer is the leading cause of cancer-associated death for women worldwide. While chemotherapy is the mainstream treatment for breast cancer, more than 50% of women undergoing chemotherapy will experience at least one chemotherapy-related adverse side effect. Sometimes, the side effects could be so severe that patients need to terminate treatment early or doctors have to reduce the chemo dosage, and this could worsen their disease. Prolonged exposure to high doses of chemotherapeutic agents could also result in resistance to chemotherapy.
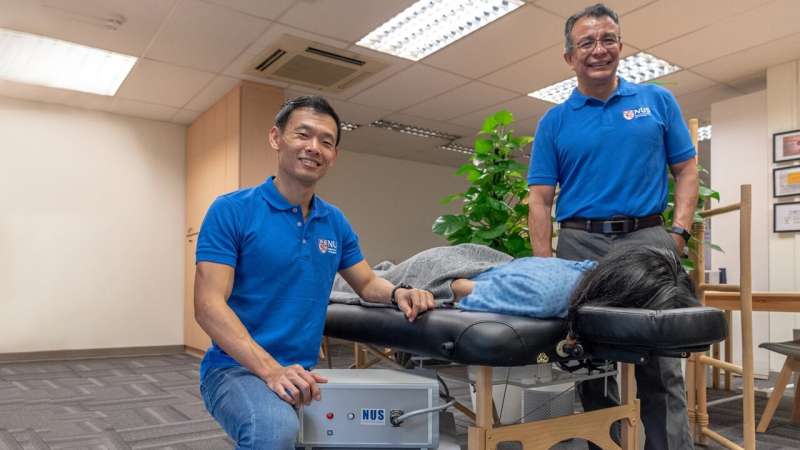
A team of researchers from the National University of Singapore (NUS) is pioneering a novel magnetic therapy—delivered using the OncoFTX System—that serves as an effective companion therapy to chemotherapy to enhance treatment outcome for breast cancer.
"Our magnetic technology stimulates cellular oxygen respiration to produce energy. In certain cancers with elevated respiratory rates—such as breast tumors—the magnetic pulses cause the cancer cells to 'hyperventilate' and die. Fortunately, the healthy tissues near the cancer are able to tolerate the increased respiratory rate, without ill consequences. Therefore, the OncoFTX System is more selective for cancer than conventional chemotherapy or radiotherapy. Importantly, this therapy is localized, non-invasive and painless," explained Associate Professor Alfredo Franco-Obregón who leads the team comprising researchers from the NUS Institute for Health Innovation & Technology as well as Department of Surgery under the NUS Yong Loo Lin School of Medicine.
Assoc Prof Franco-Obregón added, "The ultimate hope is that the combination is so effective that it reduces reliance on chemotherapy and its associated chemo side effects, as suggested by our published preclinical studies, but remains to be shown in human trials."
Each session of magnetic therapy involves exposing a breast tumor to a pulsed magnetic field at a strength of 3 milliTesla, for one hour. This field amplitude is about 50 times greater than the amplitude of the Earth's magnetic field, but 1,000 times smaller than conventional magnetic resonance imaging. The imminent safety and efficacy trials will determine the best treatment frequency for breast cancer patients.
TRPC1 expression as a screening marker
In their recent study, the NUS team discovered that cancer cells that express high levels of TRPC1—a cancer-causing gene associated with various types of cancers, such as breast cancer, pancreatic cancer, glioblastoma multiforme, lung cancer, hepatic cancer, multiple myeloma, and thyroid cancer—are more vulnerable to the magnetic therapy.
Hence, elevated TRPC1 expression could be used to identify patients who are suitable for a combination treatment involving magnetic therapy and selected chemotherapeutic agents such as doxorubicin (adriamycin).
The NUS team had also demonstrated through laboratory and preclinical studies that a combination of pulsed magnetic field exposure and chemotherapy drug doxorubicin was effective in reducing the size of breast cancer tumors.
Assoc Prof Franco-Obregón commented, "Cancer cells are inherently unstable as they are in a constant state of metabolic catastrophe. Our breast cancer magnetic signal stimulates the TRPC1-mitochondria pathway, increasing the production of oxygen free radicals and resulting in ultimate demise of cancer cells."
These research findings were published in the scientific journal Frontiers in Oncology on 24 January 2022.
Clinical trial
To further validate their findings, the research team plans to embark on a first-in-human safety trial in the second half of 2022, in collaboration with the National University Cancer Institute, Singapore (NCIS) at the National University Hospital. The one-year clinical trial is expected to involve about 30 breast cancer patients who will undergo the magnetic therapy in combination with chemotherapy.
Dr. Joline Lim, Consultant, Department of Hematology-Oncology, NCIS, said, "We observed encouraging results from preclinical studies showing improvement in local shrinkage of breast tumor. This first-in-human study will help to determine the safety of this therapy in patients, both given alone and in combination with chemotherapy. Our long-term goal is to establish its safety and efficacy in enhancing local treatment effect of chemotherapy to help patients achieve maximal shrinkage with minimal side effects."
Future research
The NUS team also plans to test the effectiveness of their magnetic therapy in other types of solid tumors—such as prostate cancer—with and without chemotherapy.
"Prostate cancer shares many similarities with breast cancer as both are primary epithelial in nature and are hormone-driven malignancies. We have also found that prostate cancer is associated with elevated TRPC1 expression. This makes prostate cancer a likely candidate for us to apply the magnetic therapy to ascertain its effectiveness," said Assoc Prof Franco-Obregón.
In the long term, the NUS team hopes their discovery will enable scientists to better optimize magnetic regimens for more effective killing of cancer cells, and in turn, translate this knowledge into effective therapies to benefit cancer patients.
More information: Yee Kit Tai et al, Modulated TRPC1 Expression Predicts Sensitivity of Breast Cancer to Doxorubicin and Magnetic Field Therapy: Segue Towards a Precision Medicine Approach, Frontiers in Oncology (2022). DOI: 10.3389/fonc.2021.783803