Patient-initiated brief admission an important complement to psychiatric outpatient care
Patient-initiated brief admission as a complement to outpatient psychiatric care is appreciated by nurses and patients, and can reduce levels of anxiety in people with emotional instability and self-harm, a new thesis from Karolinska Institutet reports.
Self-harming behavior is a serious societal problem, especially among the young. Around half of psychiatric patients and a third of Swedish upper-secondary school students have harmed themselves at least once. Self-harm is common in patients with emotional instability, often diagnosed with borderline personality disorder, and there is now a novel form of outpatient care called patient-initiated brief admission (PIBA) for this group.
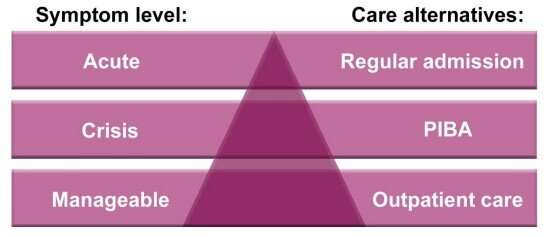
PIBA enables the patients themselves to call the psychiatric ward to initiate a brief period of inpatient psychiatric care of one to three days up to three times a month. The method was introduced in Stockholm in 2015 as a research project financed by the Swedish Research Council and led by Lena Flyckt, associate professor and psychiatrist and co-supervisor to Joachim Eckerström who has written the thesis.
Today it has spread to 18 of Sweden's 21 regions, albeit with certain variations in implementation and structure. The Center for Psychiatry Research in 2019 was tasked with developing a generic model for PIBA within the Stockholm region. The Swedish government recently instructed the National Board of Health and Welfare to draw up a set of standardized recommendations for the method nationally.
"Our focus has been to develop an intervention that can provide care at the right time, and thereby prevent patients only receiving psychiatric care once they have attempted suicide or harmed themselves in a way that requires emergency care," says Joachim Eckerström, who recently completed his doctoral thesis under supervisor and researcher Nitya Jayaram-Lindström at the Department of Clinical Neuroscience, Karolinska Institutet.
Appreciated by patients and nurses
In his thesis, Joachim Eckerström shows that nurses and patients with emotional instability were both favorably disposed to PIBA. Amongst other responses, the nurses said that the method fosters caring relationships, while the patients reported increased health-related quality of life.
"PIBA gives patients an opportunity to take time out in a secure environment when going through an unmanageable life crisis," says Eckerström. "What we find is that PIBA has a clear anxiety-mitigating effect that reduces the anxiety level of patients with emotional instability from severe to moderate after admission, and significantly increases life quality."
One of thesis' four studies also shows that PIBA seems to reduce the need for inpatient care, but the effect was not statistically significant and requires further investigation.
The diagnosis borderline personality disorder affects around 1–2% of the Swedish population; 75% of this group are women. Those affected present with a pattern of unstable relationships, severe emotional swings and uncertain self-image and identity. Some 70% of the patients with emotional instability have attempted suicide at least once in their life.
PIBA requires patients to have a previous relationship with inpatient psychiatric care and is based on an agreement between the patient and the outpatient and inpatient psychiatric services. Patient independence is encouraged, and many patients have continued to study or work in the meantime. The thesis shows that two of the challenges of PIBA are access to inpatient beds and the knowledge level of the nursing staff.
In Region Stockholm, PIBA has also been used for patients with psychosis and eating disorders, and is currently being upscaled to all patients in psychiatric care. Researchers are monitoring developments and a health-economic study on the use of PIBA for patients with emotional instability is being conducted.
"We might eventually find that the number of emergency beds can be reduced in favor of patient-initiated beds," says Eckerström. "There's a misconception that psychiatric care is stuck in a rut, but here we've developed a structured form of care that directly helps people in inpatient psychiatric care."
More information: Joachim Eckerström, Patient-initiated brief admission for emotional instability and self-harm, ISBN 978-91-8016-685-0. openarchive.ki.se/xmlui/bitstr … /10616/48081/Thesis_%20Joachim_%20Eckerstr%C3%B6m.pdf?sequence=1&isAllowed=y


















