Key blood clotting protein could be 'warning light' for severe COVID cases
A protein that could be an early indicator of severe COVID-19 has been identified and described by scientists at the University of Aberdeen.
Patients who get seriously ill following a COVID-19 infection frequently show evidence of a severe form of lung disease and in around 30% of patients blood clots are evident. Blood clots arise due to deposits of fibrin within the lung contributing to pneumonia and respiratory distress. These fibrin deposits restrict the amount of oxygen absorbed into the lung.
Patients with severe disease require oxygen support, which in very severe cases requires mechanical ventilation. In addition, blood clots are found throughout the body of those that are severely ill in both small and large vessels, frequently leading to DVT, stroke and other thrombotic complications.
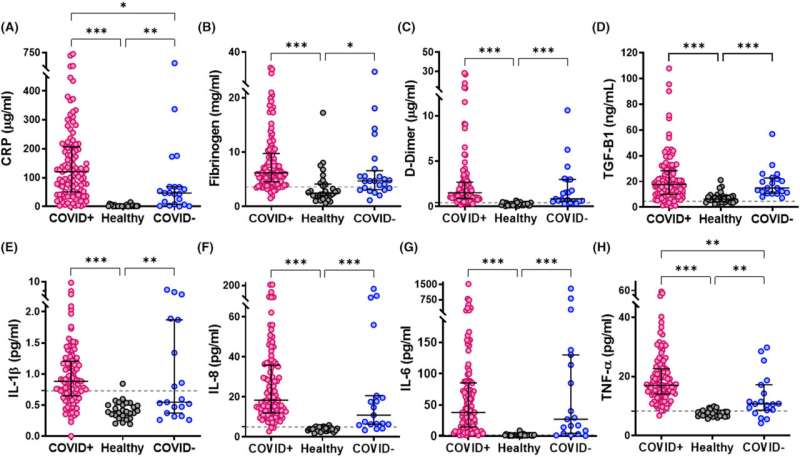
The study, published in the Journal of Thrombosis and Haemostasis, analyzed profiles of 113 patients hospitalized in Aberdeen with severe COVID-19; 24 patients with non-COVID-19 respiratory infection; and a control group with no symptoms.
The research group found that patients with COVID-19 had significantly higher levels of a protein called PAI-1 (plasminogen activator inhibitor 1) compared to those with non-COVID respiratory infections and those with no infection at all. PAI-1 acts to inhibit breakdown of fibrin in the body. As such, the high PAI-1 in COVID-19 patients prevents fibrin removal from the lung and other parts of the body, giving rise to pneumonic complications and thrombosis.
The team say the study results indicate that PAI-1 could be a potential early indicator of severe COVID-19 outcome. Not only that but the results from the group indicate that an existing clot-busting drug, Tenecteplase, could be used to treat the condition.
Lead researcher Prof. Nicola Mutch from the University of Aberdeen, said, "Our challenge is to understand why patients with severe cases of COVID-19 are so prone to the development of these clots in big and small blood vessels throughout the body.
"In this study we have identified PAI-1 as a key protein involved in the persistence of blood clots in severe COVID-19 disease. PAI-1 is associated with a poorer outcome in patients. There are existing drugs that could be utilized to promote breakdown and clearance of fibrin in the lung of those with severe COVID-19, our study shows that a PAI-1 resistant form of a clot busting agent, Tenecteplase, is superior over other drugs. Our data indicates a novel strategy to treat patients with severe COVID-19 and subsequent severe acute respiratory coronavirus infections."
More information: Claire S. Whyte et al, The suboptimal fibrinolytic response in COVID‐19 is dictated by high PAI‐1, Journal of Thrombosis and Haemostasis (2022). DOI: 10.1111/jth.15806