Quick test kit to determine a person's immunity against COVID-19 and its variants
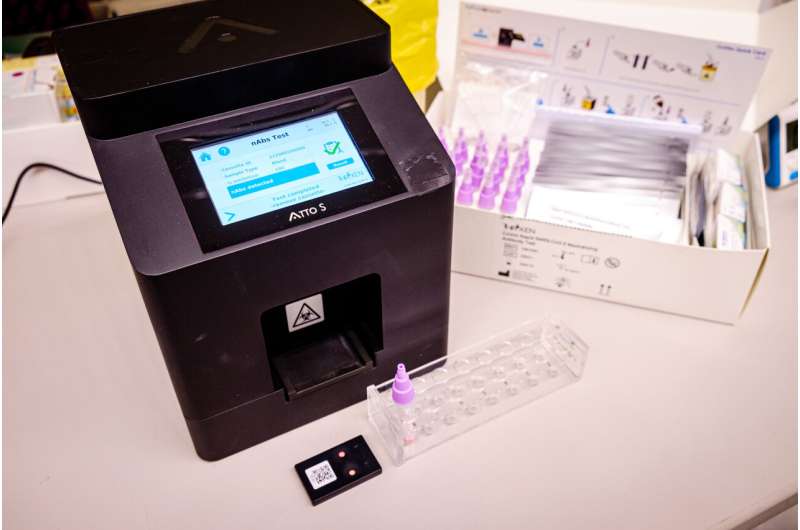
A team of scientists from the Singapore-MIT Alliance for Research and Technology (SMART), MIT's research enterprise in Singapore, and Nanyang Technological University, Singapore (NTU Singapore) has developed a quick test kit that can tell if a person has immunity against COVID-19 and its variants, based on the antibodies detected in a blood sample.
Different from ART test kits—which look for the presence of viral proteins produced during a COVID-19 infection to determine if a person is infected—this rapid point-of-care test kit is a serology test that measures antibodies made by the patient. It requires a drop of blood and takes just 10 minutes to show results, as compared to the 24 to 72 hours required for conventional laboratory testing.
The test kit detects the levels of neutralizing antibodies against SARS-COV-2, the virus causing COVID-19, and its variants such as delta and omicron, and can be easily adapted for new variants of concern and other diseases in the future.
Using a paper-based assay that is coated with chemicals that bind to antibodies in the blood sample, the test kit is low-cost, fast and has up to 93% accuracy. It paves the way for personalized vaccination strategies, where people are only given vaccinations and booster shots when necessary, depending on their variance in antibody levels and immune response.
The findings were published in the scientific journal Microbiology Spectrum by the joint team led by SMART's Antimicrobial Resistance (AMR) Interdisciplinary Research Group (IRG) and NTU's School of Biological Sciences, in collaboration with Singapore's National University Hospital (NUH) and National Center for Infectious Diseases (NCID), and Massachusetts Institute of Technology (MIT).
Fast and accurate tests to overcome challenges
Having an accurate and rapid serology test can enable governments and health care organizations to effectively manage limited vaccine resources, and address vaccine hesitancy, particularly concerning multiple booster doses.
Vaccination has been an integral component of public health strategies to tackle the COVID-19 pandemic, with 12.6 billion doses across 184 countries administered as of Sept. 9, 2022. Vaccines reduced the COVID-19 death toll by 63% within the first year of their rollout, preventing an estimated 19.8 million deaths worldwide, according to a report by the World Health Organization (WHO).
In Singapore, the Ministry of Health (MOH) estimated in February 2022 that COVID-19 vaccines had prevented 8,000 deaths during the wave of the delta variant in 2021, as well as preventing an estimated 33,000 severe cases and 112,000 hospitalizations.
However, a clinical study by the joint research team has shown that the protection offered by currently available vaccines steadily declines over three months, with varying degrees of decline across individuals. The study showed that after three months of a booster shot, the neutralizing antibody (NAb) response against wildtype and delta still remained high at medians of 91.8%, while medians against beta and gamma had dropped to 82.7 and for omicron, a large drop to 70.7%, down from 92.9%.
The emergence of novel variants with much higher transmissibility than the wild-type virus—such as delta and omicron—has exacerbated the issue of using mRNA vaccines developed based on the wildtype virus to boost immunity, especially when some current vaccines are showing reduced protection against these novel variants of concern (VoC).
In addition, vaccine hesitancy remains among limited subsets of the population, where people are wary of taking the vaccine or booster shots due to fear of side effects, further compounding the difficulty in employing a widespread vaccination strategy to build herd immunity.
To address vaccine hesitancy and efficacy of vaccination against novel variants, a personalized vaccination approach could be more effective, one which offers booster doses to individuals assessed to be more at risk, such as health care workers and the elderly.
For a personalized approach to be effective, health care workers need to be able to quickly evaluate the level of NAb response against variants at the individual level, using an easy-to-use point-of-care test kit in clinics, hospitals or vaccination centers.

Corresponding author of the paper, Professor Peter Preiser, Co-Lead Principal Investigator at SMART AMR and Associate Vice President for Biomedical and Life Sciences at NTU Singapore said, "Our team's work in the development of a rapid test kit has given us valuable insights into vaccine effectiveness and protection longevity. Our study proves that our new test kit can be a powerful tool, allowing health care organizations to screen people and determine their vaccination needs, especially against the current and upcoming variants. This will help allay some people's fears that they will be 'over-vaccinated with a booster,' since the results will inform them accurately if they are well-protected against COVID-19 or not."
Dr. Hadley Sikes, SMART AMR Principal Investigator, Associate Professor at MIT and co-corresponding author of the paper added, "Over the course of the pandemic, several large studies have shown that NAb levels against the dominant variant at the time of the study are a reliable indicator of protection from infection. Some segments of the population have low tolerance for risk of infection. The test kit we developed can provide valuable, individualized information about how quickly or how slowly a person's antibodies levels have fallen, allowing them to stay informed of their health and, whenever required, get a necessary booster dose to protect themselves."
Proven effectiveness of antibody test kit
In their research paper, the team describes a clinical study of their cellulose pulled-down virus neutralization test kit (cpVNT), a neutralizing antibody blood test designed to assess an individual's immunoprotective profile against SARS-CoV-2 and its variants.
With a drop of finger prick blood, the test kit can evaluate an individual's neutralizing antibody level against a specific COVID-19 variant within 10 minutes, making this an efficient, low-cost, and easy-to-use tool that will enable large-scale testing and can be widely deployed anywhere as part of a personalized vaccination strategy.
The test reveals the individual's level of neutralizing antibodies, which can then inform a person when a booster should be taken, and how cautious they should be about potential transmission before it is taken.
It can be administered by a layperson without medical training and does not require any specialized laboratory equipment, paving the way for large-scale testing of vulnerable subsets of the population such as the elderly.
Co-first author of the paper and former Postdoctoral Associate at SMART AMR Hoi Lok Cheng said, "This is an exciting breakthrough for us, and a continuation of our long-running work to develop efficient, low-cost, and easy-to-use NAb tests to combat the COVID-19 pandemic. As a quantitative test that can detect NAb levels specific to key variants such as delta and omicron, the cpVNT has given us valuable insights into the effectiveness of various vaccines vis-à-vis variants of concern. This test kit will also prove integral to a more personalized vaccination approach that will benefit higher-risk individuals such as the elderly and health care workers. Individuals from these communities can have their immuno-protective profile assessed on a regular basis via the cpVNT, allowing them to know when a booster dose may be appropriate or necessary. Furthermore, this test can be easily adapted to test for novel SARS-CoV-2 variants that may emerge in the future."
This research builds on years-long body of work by the SMART team. In a paper published in the medical and public health journal Communications Medicine, the team laid out the foundation for a cellulose-based vertical-flow test to detect neutralizing antibodies against SARS-CoV-2.
A separate paper published in premier chemical engineering journal Bioengineering and Translational Medicine discussed the test's effectiveness against other methods such as the pseudovirus-based virus neutralization test (pVNT) and surrogate virus neutralization test (sVNT), with favorable results.
Using clinical samples (including both whole blood and plasma) and the World Health Organization International Standard and Reference Panel for anti-SARS-CoV-2 antibody, the team established that a whole-blood test such as the cpVNT could be as informative as a plasma-only test.
As plasma- or serum-based tests require laboratory equipment to process the blood sample as well as higher quantities of blood samples to be taken, the cpVNT is therefore more resource-efficient and less invasive.
Furthermore, the cpVNT's viability demonstrates that neutralizing antibody and point-of-care tests can be successfully performed using such a format and protocol—paving the way for further development and innovation of this platform to tackle other diseases.
Further development of the test kit is underway to meet the necessary regulatory approvals and manufacturing standards for public use. The team that has developed the tests at SMART has also spun off a biotech startup, Thrixen, which is developing the test into a commercially ready product.
Key development of the rapid test was done at SMART AMR together with NTU scientists, who helped in the design of the study, providing specific reagent supplies and clinical sample collections. NUH and NCID had provided clinical sample supplies and consultation on medical use of the test, while MIT supervised the project.
More information: Hoi Lok Cheng et al, Rapid Evaluation of Vaccine Booster Effectiveness against SARS-CoV-2 Variants, Microbiology Spectrum (2022). DOI: 10.1128/spectrum.02257-22