This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Scientists improve the equation in FDA guidance predicting drug interactions
Drugs absorbed into the body are metabolized and thus removed by enzymes in several organs like the liver. The clearance rates of drugs can be increased by other drugs that increase the level of enzymes in the body. This dramatically decreases the concentration of a drug, reducing its efficacy and often leading to its failure. Therefore, accurately predicting the clearance rate in the presence of drug–drug interaction is critical in new drug development and prescription.
In terms of metabolism, drug–drug interaction is a phenomenon in which two or more drugs are taken together—one drug changes the metabolism of another drug to promote or inhibit its excretion from the body. As a result, it increases the toxicity of medicines or causes loss of efficacy.
To indirectly evaluate drug–drug interactions, pharmaceutical scientists have relied on the 110-year-old Michaelis-Menten (MM) model, which describes the reaction rate of enzymes. Although the MM equation has been one of the most widely used equations in biochemistry (it has appeared in more than 220,000 published papers), it has a fundamental limit.
The MM equation is accurate only when the concentration of the enzyme that metabolizes the drug is much lower than its MM constant (Km). Furthermore, when the enzyme concentration is increased by drug–drug interaction, the MM equation is expected to be extremely inaccurate.
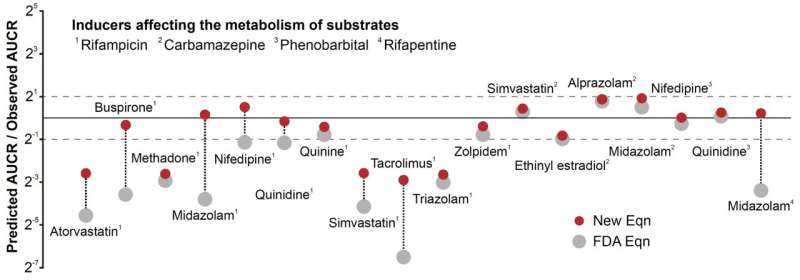
Notably, the Food and Drug Administration published a guidance in 2020 that includes an equation based on this model to predict the change in drug clearance. However, the accuracy of the equation has been highly unsatisfactory—only 38% of the predictions had less than two-fold errors. To resolve this, scientifically unjustified artificial constants have been incorporated into the equation to improve its prediction. Professor Chae Jung-woo said, "This is comparable to epicyclic orbits having to be introduced to explain the motion of the planets using the now-defunct Ptolemaic theory."

A joint research team composed of mathematicians from the Biomedical Mathematics Group within the Institute for Basic Science (IBS) and the Korea Advanced Institute of Science and Technology (KAIST) and pharmacological scientists from the Chungnam National University reported that they identified the major causes of the FDA-recommended equation's inaccuracies and presented solutions.
When estimating the gut bioavailability (Fg), which is the key parameter of the equation, the fraction absorbed from the gut lumen (Fa) is usually assumed to be one. However, many experiments have shown that Fa is less than one, obviously since it can't be expected that all of the orally taken drugs to be completely absorbed by the intestines. To solve this problem, the research team used an "estimated Fa" value based on factors such as the drug's transit time, intestine radius, and permeability values and used it to re-calculate Fg.
Also, the team used an alternative model they derived in a previous study from 2020, which can more accurately predict the drug metabolism rate regardless of the enzyme concentration, unlike the MM equation. Combining these changes, the modified equation with re-calculated Fg had a dramatically increased accuracy of about 80%, up from 38%.
"Such drastic improvement in drug–drug interaction prediction accuracy is expected to greatly contribute to increasing the success rate of new drug development and drug efficacy in clinical practice. As the results of this study were published in the top clinical pharmacology journal, it is expected that the FDA guidance will be revised according to the results of this study," said Professor Kim Jae Kyoung from the IBS Biomedical Mathematics Group.
The paper is published in the journal Clinical Pharmacology & Therapeutics.
Furthermore, this study highlights the importance of collaborative research between research groups in vastly different disciplines, in a field that is as dynamic as drug interactions.
"Collaboration between various disciplines, especially convergence research with mathematics, which is a basic science, reminded me of a proverb; going alone goes fast, but going together goes far," said Professor Kim Sang Kyum.
More information: Ngoc‐Anh Thi Vu et al, Beyond the Michaelis‐Menten : Accurate Prediction of Drug Interactions through Cytochrome P450 3A4 Induction, Clinical Pharmacology & Therapeutics (2022). DOI: 10.1002/cpt.2824