This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Social determinants of health reflected in geographical analysis of COVID-19 data
March 11 marks three years since the World Health Organization (WHO) declared COVID-19 a pandemic. As the virus spread, a pattern emerged: communities with a lower socioeconomic status tended to be disproportionately impacted.
"COVID is not just a medical outbreak, it is actually a health disparity problem," said geographer Ming-Hsiang Tsou, director of the San Diego State University Center for Human Dynamics in the Mobile Age. "Before, we knew there was a disparity, but COVID exaggerated the disparity patterns. It actually helped us reveal how vulnerable our communities are."
For example, San Diego's South Bay area has a high poverty rate and its residents experience inequitable access to health care. It was a COVID-19 hot spot throughout the pandemic, in part because it is home to many essential workers who provide for entire families.
"They are not like other, high-income people that can work from home," said Tsou. "They don't have a choice."
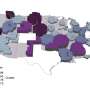
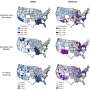
To better understand social determinants of health during the pandemic, Tsou formed an interdisciplinary team including geography graduate students and social work, statistics and sociology faculty. The researchers conducted three case studies analyzing the spatial dynamics of the disease and how they changed during five phases from April 2020 through March 2021. The first compared COVID-19 infection rates by ZIP code across San Diego County. The second extended the analysis to six large cities across the country. The third compared San Diego County data to that of other California counties.
"COVID-19 is probably the first time in human history we can monitor a disease outbreak in real-time, with data updated every single day," said Tsou. "A lot of the previous studies only took one snapshot at a time and they didn't consider that in every different wave the impact to our society—the social determinants of health—is different."
Tsou's team found that while San Diego's South Bay region was a consistent COVID-19 hot spot throughout all phases of the pandemic—reflecting persistent health disparities faced by the population—in the later phases, rural East County and Escondido became hot spots as well. In contrast, northern coastal areas such as Del Mar and Carlsbad maintained consistently low case rates. Tsou believes these spatial dynamics have implications for public health policy.
"If we can move more prevention health care resources to the South Bay area, we can resolve the COVID cases more quickly and more effectively," he said.
In San Diego County, being Hispanic, uninsured, low-income, or part of a Spanish-speaking household were all associated with higher COVID-19 rates, as were low educational attainment and living in a high-density household. These patterns held true for the most part when San Diego was compared to other counties in California, as well as all six metropolitan areas studied—from Phoenix to New York City—even though every city also had some unique factors associated with COVID-19 infections.
Tailoring policy to the needs of vulnerable groups could decrease the impact of the disease, said Tsou. That could include providing compensation for time away from work to essential workers, culturally appropriate health education around vaccines to non-English speakers, and information about free treatment options for uninsured patients.
The researchers found other important differences in COVID impacts at different stages of the pandemic. For example, the relationship between household size and infection rates grew stronger during the first four stages of the pandemic, while the proportion of teenagers and young adults infected decreased over time.
Tsou believes policymakers should take note of these temporal disease dynamics, modifying policy to align with new findings.
He said a spatiotemporal approach to data analysis could have applications beyond COVID-19.
"The future will come with a different variety of disease outbreaks, but my hope is we can build a long-term monitoring system that can analyze data every single day," he said. "If we can catch those diseases at the very early stage, public health officers can make better decisions more quickly and prevent severe illness and death in vulnerable communities."
The study is published in the Annals of the American Association of Geographers.
"While we are slowly phasing out of a public health emergency, 500 Americans are still dying each day from COVID-19," said the director of SDSU's School of Public Health, Eyal Oren, who collaborated with Tsou on another COVID-19 paper, but was not involved in this study. "The recently published paper by Tsou et al. is particularly timely in showing the degree to which social determinants of health influence the variability in COVID-19 infections."
More information: Ming-Hsiang Tsou et al, Analyzing Spatial-Temporal Impacts of Neighborhood Socioeconomic Status Variables on COVID-19 Outbreaks as Potential Social Determinants of Health, Annals of the American Association of Geographers (2023). DOI: 10.1080/24694452.2022.2149460