This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Vaccine hesitancy has become a nationwide issue: What can science do about it?
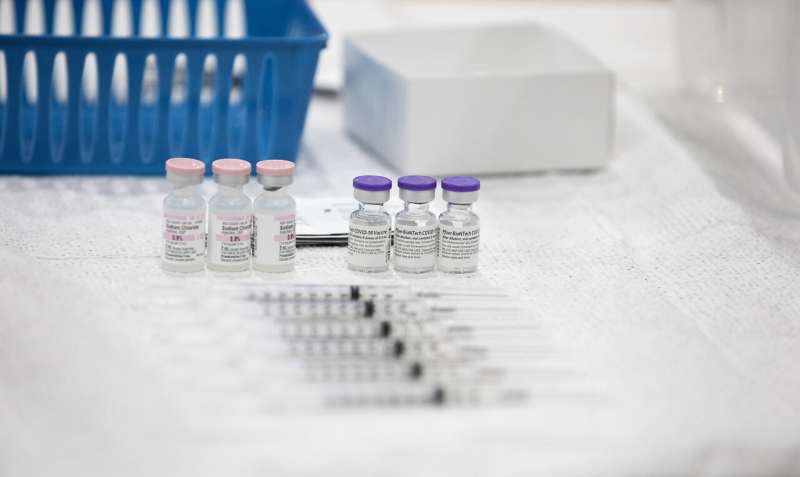
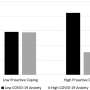
South Carolina residents were more hesitant than Americans as a whole to receive the COVID-19 vaccine during the fall of 2020, report researchers in the Department of Psychiatry and Behavioral Sciences at the Medical University of South Carolina (MUSC) in the Journal of Psychiatry Research.
The MUSC study showed that the two most important factors contributing to COVID-19 vaccine hesitancy were low levels of confidence in public health scientists and low levels of collective responsibility to prevent COVID. Postdoctoral fellow Caitlin Rancher, Ph.D., and Dean G. Kilpatrick, Ph.D., director of the National Crime Victims Research and Treatment Center, led the study.
The first step in combating vaccine hesitancy is to figure out why people are unwilling to receive vaccines, said Rancher. This will inform scientists on how to better educate the public on why these vaccines are beneficial. MUSC researchers like Rancher and Kilpatrick are stepping up to the plate and taking this challenge head on.
"It's really understanding the factors that are contributing to hesitancy," said Rancher. "It's critical because it can help us to inform public health with targeted and effective response campaigns."
To understand these factors better, the researchers surveyed a national sample of 1,450 people, excluding South Carolinians, and a state sample of 784 South Carolinians. To select recipients, they drew on the MFour Mobile Research Panel, which includes approximately 2 million people reflective of all 50 states and the District of Columbia. To participate in the survey, recipients had to have a smartphone and register for MFour's Surveys On The Go app.
"The MFour Mobile Research Panel has several advantages for this type of research due to its large size and widespread coverage of South Carolina and the U.S. and the fact that the panel is constructed to closely match the demographic characteristics of the U.S. population," said Kilpatrick.
The survey asked recipients to gauge their degrees of trust in the COVID-19 vaccine and their intentions to receive it. Researchers assessed several of these survey questions with validated multi-item measures known as the 5Cs:
- Confidence: Do I trust the science and my provider?
- Complacency: Is this vaccine necessary to my health?
- Constraints: Is the vaccine affordable and accessible?
- Risk Calculation: What is the risk of me getting sick with this disease?
- Collective Responsibility: Will getting this vaccine help others in the community?
The MUSC study found that two components of the 5C model were the driving factors for the increased hesitancy in South Carolina: confidence in science and shared collective responsibility. South Carolina residents reported lower confidence in their providers and the science backing the vaccine. Residents also felt less collective responsibility or an ethical obligation to get vaccinated to protect their community.
Focusing on these components of vaccine hesitancy will allow researchers to do a better job of educating patients and communities in vaccine science and the benefits of certain shots, said Angela Moreland-Johnson, Ph.D., a co-author of the study and an assistant professor at MUSC in the Department of Psychiatry and Behavioral Sciences. She believes a way to overcome vaccine hesitancy is to educate health professionals to help patients to understand the science and the benefits of the vaccine.
"The science and the medicine don't do a whole lot of good if people don't trust in them and trust what's being told and given to them," she said.
Although vaccine hesitancy is not new, the pandemic exacerbated the situation. And as the survey brought to light, distrust in the scientific community has grown markedly, leading to reluctance by some to accept not only the COVID-19 vaccine but even standard childhood shots.
"Globally, we're really seeing that vaccine hesitancy is contributing to a rise in cases and mortality from diseases that we thought we had a handle on," said Rancher. "For example, here, even in the U.S., in 2019, there were several measles outbreaks, where governors were declaring states of emergency."
The key takeaway from this study was that the researchers were able to determine the main drivers of COVID-19 vaccine hesitancy in South Carolina using data from the MFour Mobile Research Panel and applying the 5C model.
The MUSC researchers think that by understanding which factors are preventing people from receiving vaccines, it will allow scientists and health providers to tailor vaccine and public-education efforts specifically for those target populations. They hope that better education will lead to less vaccine hesitancy and leave the state better positioned for future outbreaks or pandemics.
More information: Caitlin Rancher et al, Using the 5C model to understand COVID-19 vaccine hesitancy across a National and South Carolina sample, Journal of Psychiatric Research (2023). DOI: 10.1016/j.jpsychires.2023.02.018