This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Research team uses genomic testing broadly for rare diseases, improves patient care
A Mayo Clinic study published in Journal of Translational Medicine has evaluated the use of genomic testing broadly for rare diseases. With the increased use of genomic testing such as multi-gene panels, exome sequencing and genome sequencing in the past decade, there is a greater opportunity to better diagnose and treat patients with rare diseases. According to the National Institutes of Health, as many as 10,000 distinct rare diseases exist and an estimated 25-30 million Americans are affected by one of them.
In the four-year Mayo Clinic study, researchers evaluated 1,152 patients with rare diseases, did genomic testing on 855 patients, and also evaluated the tested patients' family members. The overall rate where they either determined or likely determined the cause of the disease was 17.5% and as high as 66.7%, depending on the phenotype (set of observable characteristics of a person resulting from the interaction of its genotype with the environment).
As a result, 42.7% of the solved or likely solved patients had changes in their medical approaches based on the genomic testing results.
"Genomic testing has proven to be an accurate, scalable, and affordable tool for healthcare providers to diagnose rare diseases for patients with complex medical histories," says Konstantinos Lazaridis, M.D., the Carlson and Nelson Endowed Director of the Mayo Clinic Center for Individualized Medicine. "However, challenges remain for practitioners who lack the time, expertise, appropriate tools or experience to interpret genomic findings correctly."
Dr. Lazaridis explains that determining the cause of rare diseases is arduous and time-consuming and requires specific skills, including training in sequence variant interpretation. There is also a need for communication and education of the health care provider, patient, and their family.
In 2018, the Mayo Clinic Center for Individualized Medicine created the Program for Rare and Undiagnosed Diseases to integrate genomics-based care into practice, including targeted genomic testing, research and education for patients with rare diseases and their families.
The program has an integrated team and process to support physicians leading the use of genomic testing in patient care. The team of clinicians, genetic counselors and research scientists has been integral in evaluating and validating genetic variants derived from multi-gene panel testing. That has led to increased access to testing, better diagnosis, improved patient care, new knowledge and academic studies.
Additional findings from the genomic testing study
- There is a need for a multidisciplinary team to care for patients going through the genomic testing process. It is also important to understand the limitations of the different types of genomic testing.
- Genomic results may lead to the use of a targeted medication that can speedily resolve a patient's symptoms and improve their quality of life.
- Genomic testing for common diseases such as diabetes may help with diagnosis and uncover monogenic causes, which are rare, ranging from 1% to 5% of children and young adults. Confirming the diabetes diagnosis can help improve medication management and outcomes for patients and their family members.
- Including a research component in the clinical practice can help reach a definitive diagnosis, which allows for prescribing disease-specific medications or management.
- Genomic testing can help currently unaffected family members of a patient understand if they have an increased risk of developing an inherited familial disease in the future.
New service model is key to integrating genetic testing into patient care
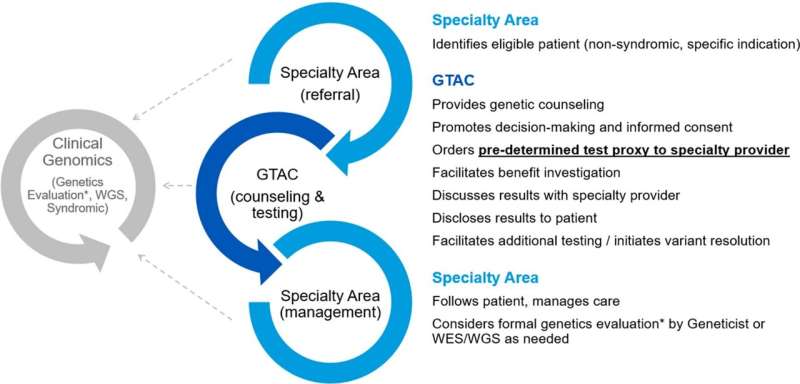
In 2020 Mayo Clinic developed the Genetic Testing and Counseling Unit to improve access to and increase the efficiency of genomic testing. The unit includes genetic counseling for patients and genomic test ordering via sub-specialty clinicians. It provides a streamlined approach to enhance access to focused genetic testing and counseling for identified conditions, reduce referral time and give just-in-time education to clinicians with limited access to genomic testing and no formal genetics training.
The researchers note that the model bridges a critical genomic testing and counseling access gap, maintaining continuity of care while providing referrals for those patients who would most benefit from further evaluation with trained medical geneticists.
They suggested that a hybrid telehealth service could increase the number of patients diagnosed, reduce the time it takes to get that diagnosis, and expand testing for rare diseases where it has been underused.
"It helps patients understand testing options' expectations and limitations, the potential effect on clinical management and the consequences to family members," says Filippo Pinto e Vairo, M.D., Ph.D., the first author of the study.
More information: Filippo Pinto e Vairo et al, Implementation of genomic medicine for rare disease in a tertiary healthcare system: Mayo Clinic Program for Rare and Undiagnosed Diseases (PRaUD), Journal of Translational Medicine (2023). DOI: 10.1186/s12967-023-04183-7