This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
proofread
Exposure to air pollution while in the womb linked to adverse changes in cell processes in newborn babies
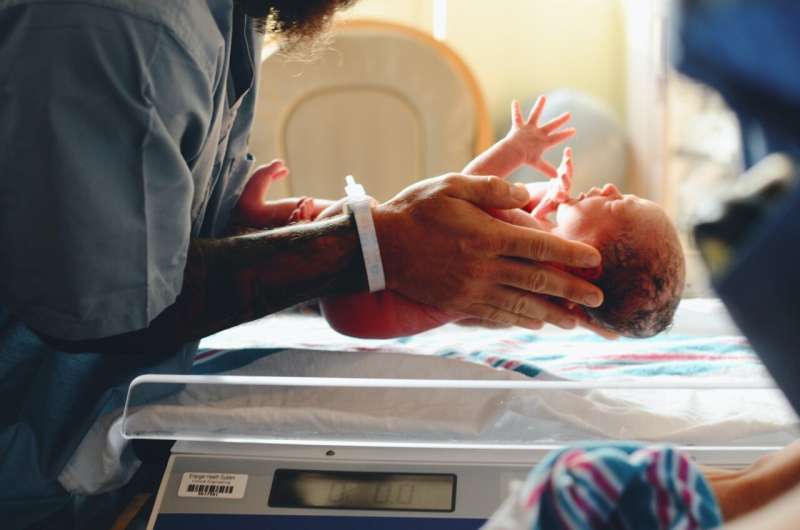
Exposure to air pollution while in the womb is linked to alterations in proteins that can be detected after a baby is born, and which affect cell processes such as autophagy, the "self-eating" of damaged cells that occurs in response to stress.
Dr. Olga Gorlanova, a research physician at the University Children's Hospital, University of Basel, Switzerland, told the European Respiratory Society International Congress in Milan, Italy, that her study also showed that healthy, newborn babies had individual and different responses to their mothers' exposure to air pollution during pregnancy. This might mean that some babies were more vulnerable to it than others. This was the case even if they were born into households in areas with relatively low levels of pollution.
Earlier work by Dr. Gorlanova and her colleagues had shown that exposure to air pollution during pregnancy could affect lung function and the immune system in newborns. In the current study, they looked at proteins involved in autophagy, aging and cell remodeling to see how prenatal exposure to air pollution could affect them.
The researchers measured 11 proteins found in the cord blood of 449 healthy newborn babies from the Bern Basel Infant Lung Development (BILD) cohort study. The BILD study, started in 1999 in Bern, aims to recruit 1000 babies by 2025. It is investigating the effects of genetics and the environment (particularly air pollution) on lung development in babies and children.
Dr. Gorlanova and colleagues measured the mothers' exposure to nitrogen dioxide (NO2) and tiny particles called PM10,which areparticulate matter measuring 10 microns or less in diameter. Vehicle emissions, tire and brake wear, and smoke are some of the sources of these pollutants. They found that NO2 and PM10 were both linked to changes in proteins involved in autophagy. Exposure to NO2 was linked to a decrease in the activity of the proteins SIRT1 and IL-8, and an increase in levels of the Beclin-1 protein.
"Our results indicate that NO2, a pollutant formed mainly from traffic emissions, is associated with increased levels of Beclin-1 protein, which is central to initiating autophagy. Exposure to higher NO2 was also linked to decreased levels of SIRT1, which is a protein that plays a protective role in stress resistance, inflammation and aging. IL-8 is a protein active in certain inflammatory cells," said Dr. Gorlanova.
"We grouped the babies into four distinct clusters according to the levels of air pollution they were exposed to while in the womb. The four clusters all had similar concentrations of the proteins being studied but had differences their exposure to NO2 and PM10 air pollution."
"One cluster had low concentrations of nine proteins, while another cluster, consisting of seven percent of all the babies, had higher levels of proteins that are involved in inflammatory and remodeling processes: IL-8 and IL-1B. Both these groups of newborns had been exposed to lower, although differing, levels of prenatal air pollution than the other two groups. Our findings suggest that healthy newborns have an individual response pattern to air pollution. We think that this may be an indication that some babies are more vulnerable to it than others."
"Additionally, our work adds to the growing body of evidence that autophagy-related mechanisms may be involved in how human cells react to air pollution. The findings are consistent with evidence from tissue and animal research. Further exploration of these mechanisms may help to better understand the deleterious effects of pollution on infants."
The researchers plan to examine whether babies with distinct protein response patterns to air pollution will suffer from more breathing problems during infancy and childhood compared to those that do not show the same protein responses.
Professor Marielle Pijnenburg, associate professor of pediatric pulmonology and head of the Department of Pediatric Respiratory Medicine and Allergology at Erasmus Medical Center, Rotterdam, The Netherlands, is head of the ERS group on pediatrics and was not involved with the research.
She commented, "This study adds to the growing body of evidence that air pollution can affect the health of children before and after they are born. It contributes to other research showing that autophagy-related mechanisms may be involved in how human cells react to air pollution. We need to know more about how these mechanisms can affect the health of lungs, and we need to understand why some newborns seem to be more susceptible to air pollution than others."
"However, we already have enough evidence from this and other studies, to be sending a message loud and clear to governments and policy-makers: air pollution damages people's health, and the effects can be seen from before birth. We should all be re-doubling our efforts to reduce air pollution as quickly and as far as possible."
"This will not only improve the health of populations and reduce costs associated with treating diseases caused by air pollution, but will also help the environment at a time when the climate emergency is becoming more and more apparent as every day passes."
More information: Abstract no: OA4941. "Prenatal exposure to air pollution affects newborns' autophagy, senescence and remodelling proteins", by Olga Gorlanova; Presented in session, "Lung structure and function across the lifespan" at 15.45-17.00 hrs CEST on Tuesday 12 September 2023. https://k4.ersnet.org/prod/v2/Front/Program/Session?e=379&session=16448