This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Study reveals disparities within NHS leadership
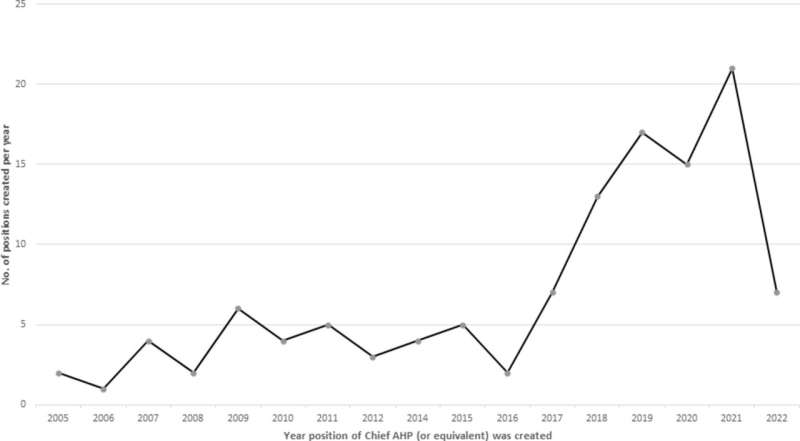
New research shows that Allied Health Professions (AHPs) are significantly underrepresented in senior leadership roles despite being the third largest workforce in the NHS.
Ranging from paramedics to podiatrists, the AHPs encompass various health care disciplines, constituting a workforce of 185,000 within the NHS.
However AHPs have historically been underrepresented in strategic leadership positions, often occupied by medical professionals. To address this, NHS England advocated for the establishment of a Chief AHP role in every Trust to harness the untapped potential of this workforce and increase diversity in leadership roles.
A recent study from Staffordshire University published in BMJ Leader provides comprehensive data on the current state of AHP strategic leadership within the NHS.
Gathering responses from 160 out of 217 Trusts and Health Boards, the study reveals that 81% of the surveyed organizations now employ a Chief AHP or equivalent. However, only 14% of these roles have a presence on the executive board of their respective Trusts or Health Boards.
The report identifies 50 diverse job titles associated with Chief AHP roles, with "Director of AHPs" (18.6%), "Lead AHP" (13.9%), and "Chief AHP" (11.6%) being the most frequently reported titles.
The findings also highlight a concerning disparity in the representation of AHP professions within senior AHP leadership, with a significant majority (70%) of these roles held by physiotherapists and occupational therapists.
Senior author Professor Nachi Chockalingam, Director of the Centre for Biomechanics and Rehabilitation Technologies, explained, "This study exposing discrepancies in AHP profession representation, the lack of standardized titles for Chief AHPs, and a significant scarcity of Chief AHPs on executive boards."
"The absence of AHP leaders in key strategic positions poses challenges, hampering the development of AHPs' leadership skills and impeding access to mentors and role models."
He added, "The inclusion of AHP leaders in planning has been proven to positively impact patient outcomes, whereas their absence can lead to missed opportunities for patients to benefit from essential AHP services."
While medical and nursing directors are required on NHS Trust executive boards in England, no comparable obligation exists for AHP representation. In contrast, Wales mandates the inclusion of a therapies and health sciences officer on boards.
The report highlights a necessity for a standardized titles for the head of AHPs. The need to mandate the presence of chief AHPs on NHS executive boards, aligning with nursing and medical roles, is also emphasized. Furthermore, identifying barriers to diverse AHP representation and promoting broader inclusion in chief AHP positions are key actions for advancing AHP leadership.
More information: Nicola Eddison et al, Exploration of the representation of the allied health professions in senior leadership positions in the UK National Health Service, BMJ Leader (2023). DOI: 10.1136/leader-2023-000737



















