This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Algorithm aids in early detection of age-related eye disease
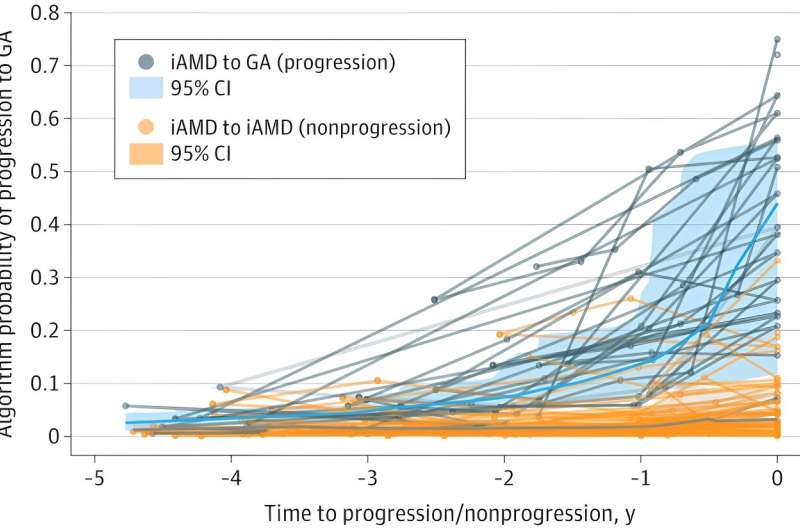
Duke University researchers created a computer program that determines, with 94% accuracy, if a person's age-related macular degeneration (AMD) will worsen within a year.
The deep learning algorithm, featured in an article published in JAMA Ophthalmology, analyzes detailed eye scans to predict if the common eye condition will progress to a more severe stage known as geographic atrophy (GA).
This faster foresight could streamline clinical trial recruitment and aid rollout of treatments designed to preserve the vision of older adults.
"Being able to predict AMD progression means we can be proactive, potentially halting its progression and improving patient outcomes," said senior study author and retina specialist Eleonora Lad, MD, Ph.D., vice chair of clinical research and associate professor at the Duke Eye Center.
Eye doctors at Duke Eye Center collaborated with Lawrence Carin, Ph.D., and Ricardo Henao, Ph.D., from Duke AI Health and the Duke Department of Electrical and Computer Engineering and global experts to study the algorithm known as DeepGAze.
"This predictive tool could transform how we screen for the disease, how often we see patients, and even when to start treatments," Lad said.
Progression from intermediate AMD to geographic atrophy represents a transition from a condition with few symptoms to one that can devastate central vision, which is needed to read, drive, and see pictures and faces.
The U.S. Food and Drug Administration recently approved two new medications that may offer a reprieve for the 1.5 million people diagnosed with geographic atrophy. Pegcetacoplan and avacincaptad pegol can slow GA's progression.
Lad was at the forefront of one of the key clinical trials for pegcetacoplan, the first FDA-approved drug for geographic atrophy. The Lancet recently highlighted Phase 3 clinical trial results confirming that injections of pegcetacoplan given once a month or every other month can curb GA lesion growth.
The algorithm, like other technology used to track diabetic retinopathy, is poised to refine the diagnostic process and help doctors pinpoint who'll benefit from treatments and ongoing care.
In JAMA Ophthalmology, researchers detail how the DeepGAze algorithm sorted through volumes of spectral-domain optical coherence tomography scans of the retina to spot which eyes would progress from intermediate stage AMD to geographic atrophy within a year.
The program used data from several U.S. clinical sites in the Age-Related Eye Disease Study (AREDS2). In all, 417 patients were involved in the study. The ability of DeepGAze to predict progression to GA within a year had a true positive rate of 0.94. In other words, it was right 94% of the time.
Even when expert graders added image annotations to identify certain conditions, a time-consuming and expensive task, the computer model did not perform significantly better than working on its own.
More information: Eliot R. Dow et al, A Deep-Learning Algorithm to Predict Short-Term Progression to Geographic Atrophy on Spectral-Domain Optical Coherence Tomography, JAMA Ophthalmology (2023). DOI: 10.1001/jamaophthalmol.2023.4659