This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
proofread
New research reveals the effects of living with antibiotic resistance
One of the first studies in the UK into what life is like for people living with antibiotic-resistant infections has revealed new ways to support those living with debilitating conditions
Research led by Dr. Ryan Hamilton, Associate Professor of Antimicrobials at De Montfort University, Leicester (DMU) is the first of its kind to provide a comprehensive understanding of the long-term impact of antimicrobial resistance (AMR) upon people's daily lives, particularly on the well-being of individuals and the support they need from health care professionals.
The resulting paper makes a number of recommendations, including the urgent provision of detailed information about AMR, its management and prevention, to patients at the point of diagnosis. The research findings, carried out in partnership with Antibiotic Research UK, the charity tackling bacterial antibiotic resistance, have been published in Scientific Reports.
Dr. Hamilton said, "Our research shows that people living with drug-resistant infections are not receiving the information and support they need from clinicians and health care providers and in our paper, we have made a number of recommendations to this effect.
"Much more needs to be done to provide accessible and understandable information to people diagnosed with drug-resistant infections, or carrying a drug-resistant microorganism long-term at the point of diagnosis.
"There is a significant lack of structured support for these people, the abandonment and isolation they feel because of lack of information and support from health care, and also a lack of support and understanding from friends and family—unlike for cancer, diabetes and respiratory disease for example; even though antibiotic resistance is already negatively impacting people with these conditions too."
The research examined, in-depth, the lives of nine participants who had been living with resistant infections or colonization for over 12 months, with a central aim to find out the key elements of experience and support needed for those living with AMR in the UK. According to a recent government report, around 150 people are diagnosed with AMR every day nationwide.
Consistent findings throughout the study uncovered a lack of support and guidance for those diagnosed with AMR infections and chronic colonization with a long-term negative impact on health and well-being—reinforcing the necessity for professional, reliable, and accessible information at the time of diagnosis—and readily available outside of health care settings.
Jonathan Pearce, chief executive officer of Antibiotic Research UK, commented, "As we've known from Antibiotic Research UK's own award-winning Patient Support Service, there is an urgent need for professional and reliable information to be available outside of core health care services, particularly through support groups and peer networks.
"More research is needed into the information and advice currently provided, as well as a focus on the impact and support needs of people living with antibiotic-resistant infections and those that care for them."
Key findings:
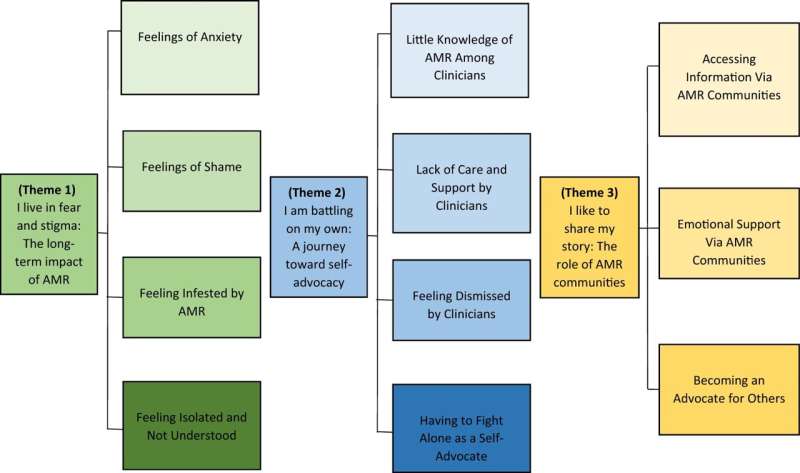
- Marginalization and empowerment: Participants described a complex experience marked by marginalization and isolation, but also moments of empowerment. Three major themes emerged: (a) Living in fear and stigma, (b) Battling on their own: A journey toward self-advocacy, and (c) Sharing their stories: The role of AMR in communities.
- Support gaps: Participants reported a lack of knowledge, information, and support from clinicians, difficulties in accessing reliable information, and a lack of understanding from family and friends. Charities and online groups emerged as crucial sources of support, addressing not only medical concerns but also mental health and well-being.
- Urgent need for information: The study emphasizes the urgent need for understandable and relatable information regarding the science of AMR, transmission, prevention, and living with AMR to be provided by clinicians and health care services around the time of diagnosis.
- Support services: Professional and reliable information should be available outside health care services, particularly through support groups provided by professionals. There is a call for more research into the impact and support needs of those with asymptomatic colonization.
Antimicrobial resistance (AMR) is the ability of microorganisms to withstand the effects of antibiotics, rendering these drugs ineffective in treating infections, posing a significant challenge to modern medicine. 148 people are diagnosed with an antibiotic resistant infection every day.
More information: Ryan A. Hamilton et al, Understanding the lived-experience and support-needs of people living with antimicrobial resistance in the UK through interpretative phenomenological analysis, Scientific Reports (2024). DOI: 10.1038/s41598-024-53814-6