This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
proofread
Continued Medicare reimbursement declines could threaten access to physicians
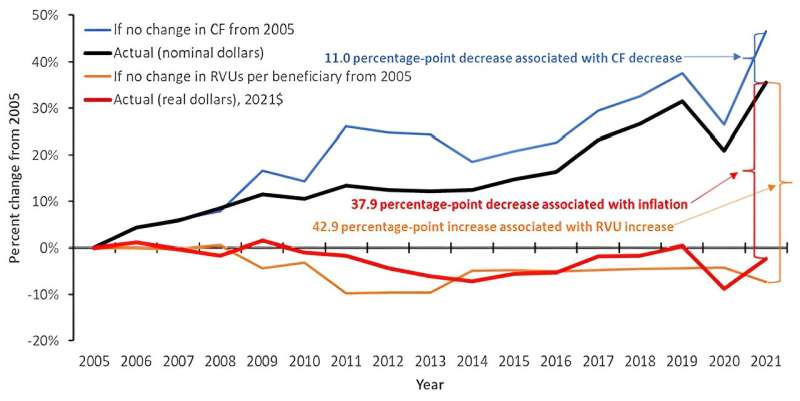
A new Harvey L. Neiman Health Policy Institute study found that physician reimbursement per Medicare patient decreased 2.3% between 2005 and 2021 when accounting for inflation, despite a concurrent increase of 45.5% in physician services to each patient.
These reimbursement trends varied widely by physician specialty (-57.6% for cardiac surgery to +189.1% for pain management). In comparison, non-physician practitioners' reimbursement per Medicare patient increased more than 3-fold over the same period.
The research, published today in INQUIRY: The Journal of Health Care Organization, Provision, and Financing evaluated changes in payments for Part B services for 100% of traditional Medicare beneficiaries between 2005 and 2021.
The study was designed to evaluate how provider reimbursement has been affected by the Medicare statutory budget neutrality requirement. Importantly, the research investigated the dynamics of the underlying factors that affect reimbursement—volume, reimbursement per service, and inflation.
Medicare reimburses clinicians based on the resource intensity of a service, measured as relative value units (RVUs). The RVUs assigned to a service are multiplied by a dollar amount per RVU (the conversion factor) to determine the Medicare payment.
"The statutory requirement for budget neutrality requires that RVUs and/or the conversion factor adjust so that Medicare expenditures do not exceed the budget as new services are introduced or as volumes of existing services increase. In other words, budget neutrality is a zero-sum game. Expansions in one area necessitate contractions elsewhere," stated Eric Christensen, Ph.D., Research Director at the Neiman Institute.
"Our study shows that physicians are now paid 2.3% less per beneficiary compared with 16 years ago as budget neutrality necessitated an offset given the substantial shift to other provider types, most notably non-physician practitioners."
Although the research found that across all medical providers and suppliers, payments per beneficiary increased by 9.9%, payments to non-physician practitioners (e.g., nurse practitioners) increased by 206.5%, while payments to limited-license physicians (e.g., podiatrists) increased by 16.3% and payment to medical suppliers increased 44.4%.
While some physician specialties experienced reimbursement growth, sixteen physician specialties experienced reimbursement declines. Of these, thirteen experienced reimbursement declines despite higher volumes per beneficiary. These included psychiatrists, cardiologists, urologists, OB/GYN, internal medicine, internists, pulmonologists, radiologists, gastroenterologists, and anesthesiologists, among others.
"Whether a specialty experienced a per beneficiary reimbursement decline or not was a function of changes in health care consumption per beneficiary and how that compared with inflation-adjusted declines in the conversion factor," stated Gregory Nicola, MD, Executive Leadership, Hackensack Radiology Group and Chair, ACR Economics Commission.
"We found that specialties would have to increase their volume of services by 50.7% per beneficiary to maintain the same per beneficiary reimbursement over the 2005-2021 period."
"While reducing physician payments can help to contain Medicare expenditures, it may also lead to unintended consequences for patients," stated Joshua Hirsch, MD, Neiman Institute Affiliate Senior Research Fellow and Vice Chair Procedural Services, Massachusetts General Hospital.
"Continued decline of Medicare reimbursement relative to reimbursement by private insurance incentivizes providers to favor privately insured patients. Our study pinpoints the extent to which real decreases in reimbursement are occurring despite greater consumption of care. We hope this study will motivate policymakers to find a solution that inures to the benefit of the Medicare-insured population who are at risk for diminishing access to care."
More information: Eric W. Christensen et al, Medicare Volume Growth and Shift in Payments From Physicians to Non-Physician Practitioners Under Statutory Budget Neutrality, INQUIRY: The Journal of Health Care Organization, Provision, and Financing (2024). DOI: 10.1177/00469580241249076