This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
reputable news agency
proofread
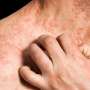
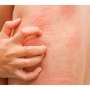
Antihypertensives linked to eczematous dermatitis in seniors, study finds
Antihypertensive drugs are associated with an increased risk for eczematous dermatitis in older adults, and the effect sizes are largest for diuretics and calcium channel blockers, according to a study published May 22 in JAMA Dermatology.
Morgan Ye, M.P.H., from the University of California in San Francisco, and colleagues examined whether antihypertensive drug use is associated with eczematous dermatitis in a longitudinal cohort study of individuals aged 60 years and older without eczematous dermatitis at baseline.
The researchers found that the overall prevalence of eczematous dermatitis was 6.7% among 1,561,358 older adults during a median follow-up of six years. The incidence of eczematous dermatitis was higher among those receiving versus those not receiving antihypertensive drugs (12 versus 9 of 1,000 person-years of follow-up).
Participants who received any antihypertensive drugs had a significantly increased risk for any eczematous dermatitis in adjusted analyses (hazard ratio, 1.29). When assessing each antihypertensive drug class individually, the largest effect sizes were seen for diuretics and calcium channel blockers, while the effect sizes were smallest for angiotensin-converting enzyme inhibitors and β-blockers (hazard ratios, 1.21, 1.16, 1.02, and 1.04, respectively).
"Although additional research is needed to understand the mechanisms underlying the association of antihypertensive drug use and eczematous dermatitis, these data could be helpful to clinicians to guide clinical management when an older patient presents with eczematous dermatitis," the authors write.
More information: Morgan Ye et al, Antihypertensive Medications and Eczematous Dermatitis in Older Adults, JAMA Dermatology (2024). DOI: 10.1001/jamadermatol.2024.1230
© 2024 HealthDay. All rights reserved.