This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Gestational diabetes: Research identifies new subgroups that improve personalized therapy
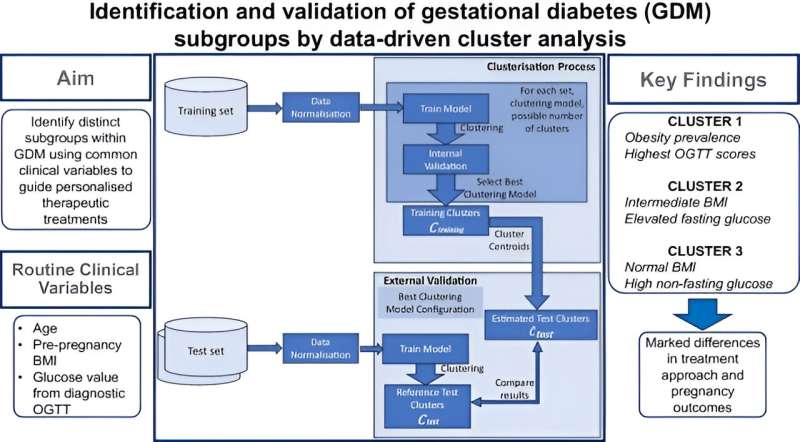
Patients with gestational diabetes show different disease progressions and therefore require personalized treatment measures. An international research team led by MedUni Vienna has now identified three subgroups of the disease with different treatment needs. The results of the study, recently published in the journal Diabetologia, could improve our understanding of gestational diabetes and significantly advance the development of personalized treatment concepts.
As part of the study, scientists from MedUni Vienna, in collaboration with colleagues from Charité—Universitätsmedizin Berlin and the Consiglio Nazionale delle Ricerche Padua, analyzed certain data from 2682 women with gestational diabetes (GDM) that had been routinely collected at MedUni Vienna and Charité between 2015 and 2022.
Using cluster analyses, a machine learning method, the patients were divided into different groups based on routine parameters such as age, body mass index (BMI) before pregnancy and blood glucose values from an oral glucose tolerance test (OGTT).
"This allowed us to clearly identify three clusters with different treatment requirements," reports study leader Christian Göbl (Department of Obstetrics and Gynecology, MedUni Vienna). "We also saw that different pregnancy complications occur at different rates in the individual subgroups."
Routine data for individualized treatment decisions
The first subtype includes women with the highest blood glucose levels, a high prevalence of obesity and the highest need for blood glucose-lowering medication. The second subgroup consists of women with a medium BMI and elevated fasting blood glucose levels. Women with normal BMI but elevated blood glucose levels after the OGTT were summarized in the third subtype.
"The patients in the subgroups we identified showed remarkable differences in terms of the need for glucose-lowering medication and treatment modalities such as rapid-acting versus intermediate or long-acting insulin," says Göbl. He points out the enormous clinical relevance of the study results, which lay the foundation for further research to develop optimal treatment strategies for each subgroup.
The newly created model for this is based on machine learning, an area of artificial intelligence that can derive predictions and decisions from data.
"In this case, only a few parameters are required that are always available in the clinical routine for gestational diabetes anyway. This means that patients can receive even more specific and individualized advice and treatment and the risk of complications for mother and child can be further reduced," says Göbl.
More information: Benedetta Salvatori et al, Identification and validation of gestational diabetes subgroups by data-driven cluster analysis, Diabetologia (2024). DOI: 10.1007/s00125-024-06184-7