This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Study finds the LGBTQI+ population have less access to health care, worse health outcomes, less insurance
Members of the LGBTQI+ population experience less access to health care, worse health outcomes, and higher rates of uninsurance than their counterparts, research has shown. To expand coverage and address health care disparities affecting LGBTQI+ populations, some U.S. lawmakers have proposed lowering the Medicare eligibility age from 65 to 60.
In a new study, published in JAMA Health Forum, Yale researchers evaluated whether this would have a meaningful impact on LGBTQI+ health equity.
Using data from the largest nationwide annual health survey—conducted between the years 2014 and 2021—the researchers compared data from individuals who identified as heterosexual with data from those identifying as lesbian, gay, bisexual, or "other" (per the survey options). Nearly 928,000 individual respondents, ages 51 to 79, were included in the study.
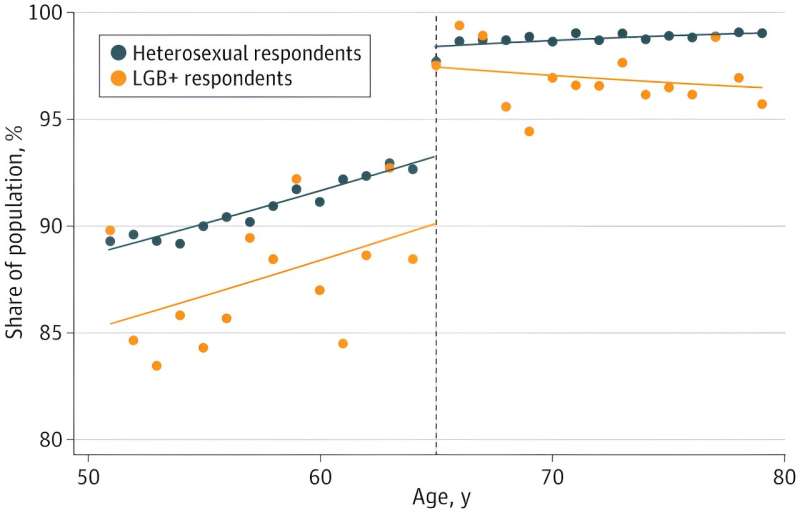
The researchers found that aging into Medicare led to increases in health insurance coverage rates, access to health care, and health for all groups. But improvements in insurance coverage and health care access, respectively, were stronger for heterosexual individuals than for LGB+ respondents.
Among LGB+ individuals, only self-reported health showed larger gains. However, when the researchers repeated the analysis on a subset of individuals in U.S. states with the greatest LGBTQI+ disparities, Medicare coverage benefited LGB+ individuals more than heterosexual respondents in coverage, access, and health status.
"This tells us that while Medicare access has positive effects, lowering the age of eligibility alone is likely not sufficient to overcome the structural and interpersonal forms of discrimination that affect LGBTQI+ populations nationally and may most benefit LGBTQI+ individuals living in states with the highest disparities," said Kyle Gavulic, lead author of the study and an M.D.-Ph.D. student at Yale School of Medicine and Yale School of Public Health.
"Additional interventions will be needed for larger, more widespread improvements to LGBTQI+ health equity."
More information: Kyle A. Gavulic et al, Medicare Eligibility and Changes in Coverage, Access to Care, and Health by Sexual Orientation and Gender Identity, JAMA Health Forum (2024). DOI: 10.1001/jamahealthforum.2024.1756