New radar better treats mobile tumors
A cancer forms and the battle begins. However, when the tumor floats freely, the disease claims an unfair advantage.
Changzhan Gu, a Texas Tech doctoral student from the Department of Electrical and Computer Engineering, has set out to level the playing field. His new radar will help make treatment safer, more effective and more comfortable for the patients with floating tumors. And his work, under the supervision of assistant professor Changzhi Li, already has won awards at two premier conferences.
“The project utilizes radar sensor technology for biomedical applications of respiratory gating and tumor tracking,” Gu said. “It is a brand-new technology to deal with mobile tumors.”
Take lung cancer, for example. At approximately 3 million deaths annually, it is one of the most fatal cancers worldwide. If the tumor is floating, it then becomes a moving target. Compound that with a patient’s breathing and targeted radiation treatments become exponentially more difficult.
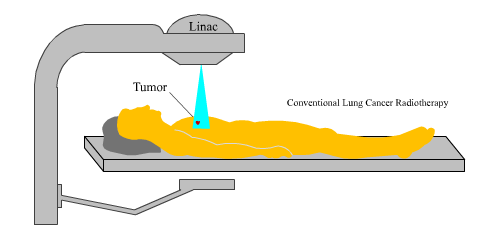
The primary device used to provide external beam radiation treatments to a patient is called a linear accelerator (LINAC). This machine delivers high-energy X-rays to the tumor, regardless of its location on the body. Ideal conditions would dictate that the tumor hold still while the concentrated beam is at work. So in the case of a floating tumor, specialists are forced to treat larger areas to compensate for the movement. While effective, it may damage healthy tissue surrounding that tumor.
To minimize the damage, specialists use respiration-gated radiation therapy, a promising treatment modality that precisely delivers a prescribed dose of radiation to floating tumors. Respiration-gated radiation therapy is only effective when the tumor is in a predefined gating window. This is accomplished when the LINAC is synced with the patient’s breathing pattern, so that radiation may be switched on and off as the tumor passes through the beam. The treatment becomes even more efficient when the patient is able to establish a steady rhythm through coached breathing, or verbal cues that let the patient know when to inhale and when to exhale. This reduces the volume of tissue irradiated, so it is safer and results in fewer side effects and complications, which in turn produces better outcomes.
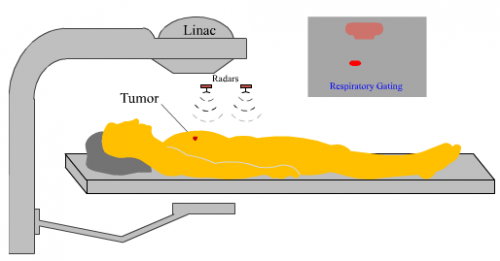
But as impressive as this technology is, it also has its downfalls. For specialists to be able to monitor the patient’s respiration in real time, they must place infrared markers to signal the machine when to turn on and off.
“Internal markers are intrusive and can produce side effects,” Gu said. “External markers are uncomfortable and lack accuracy.”
To help combat the discomfort, Gu has developed a non-contact Doppler radar that better measures respiration signals during respiration-gated radiation therapy. Analysis of the measured signal from Gu’s device has proven to be more sensitive and more accurate, plus it requires no markers and sends the data back to a computer wirelessly. The radar is even sensitive enough to sense a disruption in the normal breathing pattern, such as a cough.
“At one milliwatt, the signal is also remarkably low power,” Gu said. “It is actually less than a cell phone.”
Gu’s research papers “Doppler Radar Respiration Measurement for Gated Lung Cancer Radiotherapy” and “Radar Motion Sensing for Accurate Tumor Tracking in Radiation Therapy” has won Best Paper Awards at two premier Institute of Electrical and Electronics Engineers conferences. And he has since filed an invention discloser with the Texas Tech University Office of Technology Commercialization of radar sensor for lung cancer treatment and is taking steps toward filing a provisional patent application before the end of the year.
This research is in collaboration with the Texas Tech University Health Sciences Center, Southwest Cancer Center and the Office of Technology Commercialization.















