Antidote for cocaine overdose shows promise in lab tests
Scientists at The Scripps Research Institute have shown that an injectable solution can protect mice from an otherwise lethal overdose of cocaine. The findings could lead to human clinical trials of a treatment designed to reverse the effects of cocaine in case of emergency. Cocaine is involved in more than 400,000 emergency-room visits and about 5,000 overdose deaths each year in the United States.
The findings, reported recently in the journal Molecular Pharmaceutics, demonstrate the therapeutic potential of a human antibody against cocaine.
"This would be the first specific antidote for cocaine toxicity," said Kim Janda, PhD, senior author of the report. A pioneer in the field of vaccines against drugs of abuse, Janda is the Ely R. Callaway, Jr. Chair in Chemistry, a professor in the Department of Immunology and Microbial Science, and director of The Worm Institute for Research and Medicine, all at Scripps Research. "It's a human antibody so it should be relatively safe, it has a superior affinity for cocaine, and we examined it in a cocaine overdose model that mirrors a real-life scenario," he said.
Janda and his laboratory colleagues have been developing candidate vaccines against cocaine, heroin, nicotine, and even Rohypnol, the "date-rape" drug. But most of these have been active vaccines—solutions of drug-mimicking molecules that provoke a long-term antibody response against a drug, greatly reducing its ability to reach the brain. These are potentially useful against addiction and relapse, but take weeks to stimulate an effective antibody response and thus are of limited value in drug overdose emergencies, which require a fast-acting antidote. Cocaine is a leading cause of illegal-drug overdoses in developed countries; it can cause hyperthermia, irregular heartbeats, seizures and death.
One possibility for an antidote is a "passive" cocaine vaccine, a ready-made solution of antibodies much like those used to treat snakebite. As Janda and his colleagues have shown in previous research, injected drug-specific antibodies can swiftly remove drug molecules from the bloodstream. This immediately reduces a drug's direct effects on the heart and nearby organs, but it also pulls the drug from the organ where it does the most damage—the brain. If the drug molecules are small enough to cross the blood-brain barrier, the sudden lowering of their bloodstream concentration causes them to diffuse rapidly out of brain tissue.
Cocaine molecules are small enough to diffuse this way, and in 2005 Janda and his lab reported that injections of a mouse-derived anti-cocaine antibody, GNC92H2, could keep mice alive despite cocaine doses that killed unprotected mice. Mouse antibodies are not ideal for use in humans, though; they are "foreign" enough that human immune systems eventually develop a reaction against them.
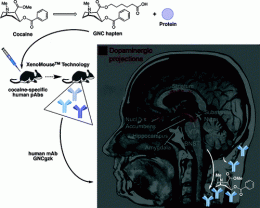
In the new study, Janda and Jennifer B. Treweek, PhD, a research associate in Janda's laboratory, used a genetically engineered mouse that can produce fully human antibodies against cocaine molecules. The best of these antibodies, GNCgzk, showed ten times the cocaine-binding affinity of GNC92H2, the molecule in the 2005 study.
In a preliminary test, the scientists showed an injection of GNCgzk antibodies 30 minutes before an injection of a lethal cocaine dose greatly reduced the signs of overdose—such as awkward movements and seizures—and kept all treated mice alive. By contrast, about half of untreated mice and 15 percent of GNC92H2-treated mice died.
In a test that better simulated a real-life emergency situation, mice were first given a cocaine overdose, and three minutes later were infused with GNCgzk. About half of untreated mice were killed by such a dose. While GNC92H2 reduced that rate to about 28 percent, the new GNCgzk antibodies reduced the mortality rate further, to 20 percent.
More strikingly, a stripped-down version of GNCgzk—F(ab')2-gzk, which contains only the antibody's cocaine-binding segments—reduced the mortality to zero, as well as significantly reducing overdose signs such as seizures. It also did so at a much smaller, clinically feasible dose than GNC92H2's. "There was a reversal of the signs of cocaine toxicity within seconds of the injection," said Treweek.
Janda and Treweek are now trying to find ways to produce their F(ab')2-gzk antidote economically and in large quantities. "If we can do that, then there would be no reason not to push it into clinical trials," Janda said.
He notes that such a treatment could be useful not only in reducing the immediate effects of an overdose, but also in preventing near-term relapses. "A lot of people that overdose end up going back to the drug rather quickly," Janda said, "but this antibody would stay in their circulation for a few weeks at least, and during that time the drug wouldn't have an effect on them." Likewise, this antibody could be administered to patients in addiction recovery or detox programs as a prophylactic treatment to supplement other medications, such as antidepressants, and counseling. An acute relapse during this recovery period would be immediately nullified by the antibody dose that is already in circulation.
More information: “An Antidote for Acute Cocaine Toxicity” Mol. Pharmaceutics, 2012, 9 (4), pp 969–978 DOI: 10.1021/mp200588v
Abstract
Not only has immunopharmacotherapy grown into a field that addresses the abuse of numerous illicit substances, but also the treatment methodologies within immunopharmacotherapy have expanded from traditional active vaccination to passive immunization with anti-drug monoclonal antibodies, optimized mAb formats, and catalytic drug-degrading antibodies. Many laboratories have focused on transitioning distinct immunopharmacotherapeutics to clinical evaluation, but with respect to the indication of cocaine abuse, only the active vaccine TA-CD, which is modeled after our original cocaine hapten GNC,(1) has been carried through to human clinical trials.(2) The successful application of murine mAb GNC92H2 to the reversal of cocaine overdose in a mouse model prompted investigations of human immunoglobulins with the clinical potential to serve as cocaine antidotes. We now report the therapeutic utility of a superior clone, human mAb GNCgzk (Kd = 0.18 nM), which offers a 10-fold improvement in cocaine binding affinity. The GNCgzk manifold was engineered for rapid cocaine clearance, and administration of the F(ab′)2 and Fab formats even after the appearance of acute behavioral signs of cocaine toxicity granted nearly complete prevention of lethality. Thus, contrary to the immunopharmacotherapeutic treatment of drug self-administration, minimal antibody doses were shown to counteract the lethality of a molar excess of circulating cocaine. Passive vaccination with drug-specific antibodies represents a viable treatment strategy for the human condition of cocaine overdose.















