Plants provide accurate low-cost alternative for diagnosis of West Nile Virus
(Medical Xpress)—While the United States has largely been spared the scourge of mosquito-borne diseases endemic to the developing world—including yellow fever, malaria and dengue fever—mosquito-related illnesses in the US are on the rise. One pathogen of increasing concern in the U.S. is an arbovirus known as West Nile.
Now Qiang "Shawn" Chen, a researcher at Arizona State University's Biodesign Institute and a professor in the College of Technology and Innovation has developed a new method of testing for West Nile, using plants to produce biological reagents for detection and diagnosis.
The new research, conducted by Chen and his colleagues at the Center for Infectious Diseases and Vaccinology recently appeared in the Journal of Biomedicine and Biotechnology.
"One critical issue in WNV diagnosis concerns the difficulty of distinguishing WNV infection from other closely related diseases, such as St. Louis encephalitis and dengue fever, due to the cross-reactivity of antibodies among flaviviruses," Chen says. "It is important to develop better diagnostic tools with enhanced accuracy for both treatment and diagnostic purposes."
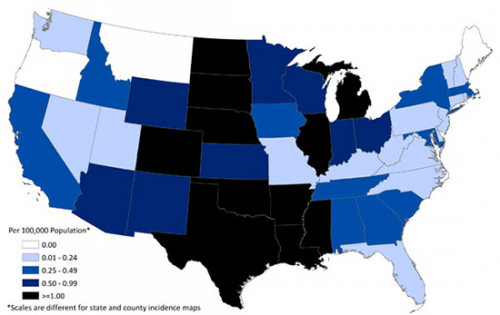
Thus far, the 2012 outbreak of West Nile in the United States is on track to be one of the worst on record. According to the Center for Disease Control, 48 states have reported West Nile virus infections in people, birds, or mosquitoes as of October 9th of this year.
To date, 4,249 cases of West Nile virus disease have been reported in humans, including 168 deaths. Of these cases 2,123 (50 percent) appeared in the more severe or neuroinvasive form of the disease, causing meningitis and encephalitis, while 2,126 cases were classified as non-neuroinvasive.
These figures represent the highest number of West Nile cases reported to the CDC since 2003, with nearly 70 percent reported from eight states: Texas, California, Louisiana, Mississippi, South Dakota, Michigan, Oklahoma, and Illinois. Over a third of total cases have been reported from Texas.
The alarming upswing in West Nile cases coupled with their broad geographic distribution demand new techniques for both diagnosis and treatment. Chen and his colleagues have been exploiting the power of plant biotechnology to achieve these goals.
Earlier, Chen's group developed the first successful plant-derived therapeutic to combat West Nile post-infection, reporting their results in the Proceedings of the National Academy of Science. The current study advances efforts to create a diagnostic test for West Nile that will overcome barriers of existing methods, including limited accuracy, prohibitive cost and scalability.
In nearly all cases, West Nile is transmitted to humans through the bite of an infected mosquito. Mosquitoes acquire the virus after feeding on infected birds. The virus then migrates to the mosquito's salivary glands, from which it may be injected into humans and animals. There, it can multiply and produce characteristic symptoms of West Nile disease. These may present as flu-like malaise including fever and chills, headaches, fatigue and pain in muscles and joints. Symptoms typically last three to six days, but may persist for weeks.
In around 1 in 150 WNV cases, individuals develop infections of the brain (encephalitis) or surrounding tissue (meningitis), often producing severe headache, fever, stiffness, confusion, convulsions, coma, tremors, muscle weakness and paralysis. Those with neurologic involvement may require weeks of hospitalization and may suffer permanent health effects including muscle weakness and paralysis. Around 10 percent of people with WNV encephalitis die.
Faced with the growing threat of mosquito-borne epidemics, researchers like Chen stress the necessity of developing rapid, low-cost platforms for diagnosis of West Nile. Traditionally, cell cultures from serum, cerebrospinal fluid or tissues have been examined but the short viremic phase and low viral count of WNV in blood and spinal fluid limit the sensitivity and accuracy of such tests. Protein-based methods like ELISA have become standard tests for West Nile, yielding better results but at considerably higher cost and with limited scalability.
In the current study, plants were exploited for their ability to produce large volumes of proteins that can be used for diagnostic testing. As Chen explains, proteins produced in this way traditionally require a lengthy time period before transgenic plant lines can be established. By contrast, the new method, which makes use of plant viral-based vectors like Tobacco Mozaic Virus and Gemini Virus, relies on the ability of plants to transiently express particular target genes, yielding the desired protein in 1-2 weeks.
The technique provides the speed and flexibility of a bacterial gene expression system while permitting the posttranslational modifications of proteins afforded by mammalian cell culture approaches.
Chen's group used plant transient expression systems to produce two varieties of protein reagents useful for the detection and diagnosis of WNV—one a recombinant antigen and one a monoclonal antibody. High expression levels of both reagents were observed in two kinds of plants: Nicotiana benthamiana (a close relative of tobacco) and lettuce. The two reagents may be readily purified to greater than 95 percent and retain their native functionality and specificity.
The production of plant-derived antigens and monoclonal antibodies offers an attractive alternative to the use of mammalian, insect or bacterial cell cultures and demonstrates the capability of plants to provide accurate and flexible diagnostic reagents not only for WNV but a broad range of arboviruses affecting human health.
"Our test will improve the accuracy of diagnosis, leading to the proper treatment of patients affected by WNV," Chen says. "The plant-derived monoclonal antibody we examined is not only low-cost, but highly specific for WNV antigen and does not recognize antigens from other flaviviruses." Chen further notes that application of this research will ultimately allow a broad range of WNV surveillance capabilities, from clinical diagnosis to global distribution patterns in wild bird and mosquito populations.
West Nile Facts
The West Nile Virus (WNV) is an arbovirus belonging to the Flavivirus genus of the Flaviviridae family
Mosquitoes that have acquired the virus from infected birds transmit WNV.
First identified in the Eastern Hemisphere and widely distributed in Africa, Asia, Europe and the Middle East, WNV entered the Western Hemisphere in 1999, via New York City.
Since its American debut, WNV has infected over 30,000 people with severe forms of the disease, with an untold number of additional cases remaining undiagnosed.
Infection with WNV can be asymptomtic or can lead to West Nile fever or severe West Nile disease.
Around 20 percent of people who become infected with WNV will develop West Nile fever, with symptoms including fever, headache, exhaustion and body aches, occasionally with a skin rash (on the trunk of the body) and swollen lymph glands. The illness can last from a few days to several weeks.
The symptoms of severe WNV disease—also known as neuroinvasive disease, including West Nile encephalitis or meningitis or West Nile poliomyelitis— include headache, high fever, neck stiffness, stupor, disorientation, coma, tremors, convulsions, muscle weakness, and paralysis.
Approximately 1 in 150 people infected with WNV develop a more severe form of disease. While serious illness can occur in people of any age, those over 50 as well as individuals with compromised immunity (including transplant patients) are at the highest risk for severe illness following WNV infection.
The incubation time for WNV is typically 2 to 15 days. It is believed that infection confers lifelong immunity to the virus.
This year (2012) has seen a serious uptick in West Nile cases and will go on record as among the most severe in terms of case numbers.
According to Scientific American, a mild winter and a hot, dry summer have contributed to the rapid spread of WNV across the U.S. this year. Climate change has been implicated as a factor exacerbating the spread of WNV.
The susceptibility to severe symptoms of WNV disease appears linked to genetic traits. Further, advanced age is one of the primary risk factors for severe neurological disease, long-term morbidity and death.
Plant production for diagnostic protein reagents may easily be scaled up to suit existing need, as in the case of a sudden WNV epidemic.
Plants are ideal protein bioreactors, due to their capacity to produce large volumes or proteins at low cost and their ability to make appropriate posttranslational modifications of proteins.
Currently, there is no vaccine against WNV, nor effective therapeutics approved for human use. The best tactics of prevention are:
More information: Journal of Biomedicine and Biotechnology Volume 2012 (2012), Article ID 106783, 10 pages doi:10.1155/2012/106783















