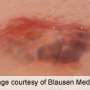
Asthma drug found highly effective in treating chronic, severe hives and itch
An international team of researchers has found that a once-a-month, high-dose injection of a commonly used asthma drug is highly effective in treating teens and adults chronically afflicted with hives and severe, itchy rash. The drug, omalizumab, was tested on 323 people at 55 medical centers for whom standard antihistamine therapy failed to quell their underlying, allergy-like reaction, known as chronic idiopathic urticaria or chronic spontaneous urticaria.
"Physicians and patients may now have a fast, safe and well-tolerated treatment option to consider before prescribing even more antihistamines, which can be highly sedating," says Sarbjit (Romi) Saini, M.D., a Johns Hopkins allergist and immunologist, and study co-investigator. The research team's findings are scheduled to be published in The New England Journal of Medicine online Feb. 24, to coincide with their initial presentation at the annual meeting of the American Academy of Allergy, Asthma & Immunology in San Antonio, Texas.
Participants in the study, which ran from 2009 to 2011, were mostly women and between the ages of 12 and 75. Each was randomly assigned to take one of three dosing regimens of omalizumab, or placebo, after which they were monitored through regular checkups for four months. Neither researchers nor participants were aware of what specific dose was being taken by which subjects during the study.
All study participants had chronic hives and rash for at least six months, with many having suffered from the condition for more than five years. All had continued to experience hives or a severe itchy rash for a full week while taking antihistamines.
"Patients suffering with this condition need more and better treatment options because chronic hives and rash are profoundly hard to treat and can be very debilitating," says Saini, an associate professor at the Johns Hopkins University School of Medicine. Saini, who has studied omalizumab since 2005, points out that fewer than half of those treated respond to traditional drug treatments with antihistamines.
Saini says the new study results offer substantial evidence that this first injection treatment option not only works, but does so more safely than other drugs, such as corticosteroids and the immunosuppressant cyclosporine, which carry risk of potentially severe and toxic side effects, including high blood pressure, bone thinning and even infection. By contrast, headache was the most severe side effect observed with omalizumab therapy. No study participants died or suffered anaphylactic shock, or had to withdraw because of any adverse effects or events.
According to Saini, chronic idiopathic urticaria affects some 3 million Americans, and may or may not involve swelling, with twice as many women as men suffering from these often socially isolating conditions. Saini says some patients experience such severe swelling of their eyes, hands, face, lips and throat that they have difficulty breathing. Some refuse to leave home, losing several days at a time away from work during flare-ups.
In the study, the team of American and European researchers injected a 300-milligram dose of the drug, sold under the brand name Xolair, once a month for three months. Saini says initial relief from symptoms was quick and occurred after a week. After three months, 53 percent of people experienced a total elimination of all hives and 44 percent had no further incidents of hives or itch. Lower doses of the drug, at 150 milligrams and 75 milligrams, and the placebo (or 0 milligrams) proved half as effective as the next larger dose, or had almost no effect at all, researchers say.
Saini, who also serves as director of Johns Hopkins' medical fellowship training program in allergy and clinical immunology, had conducted earlier research on the test doses, which he says are different from those used in omalizumab therapy for asthma. Single, uniform doses of omalizumab can be used to treat hives, whereas dosing for asthma is calculated based on the patient's weight and blood levels of IgE antibodies, known to play a key role in allergic reactions.
Researchers say it remains unclear as to precisely how omalizumab, first approved in the United States in 2003 as a treatment for severe asthma, stops the runaway allergy-like reactions underpinning chronic hives and itching. What is known, he says, is that omalizumab binds up free IgE circulating in the body, and lowers the number of IgE receptors on other histamine-carrying immune system cells. Saini says that in a typical allergic reaction, allergens, such as pollen and dust particles, bind to IgE receptors that sit on these immune system cells. This process quickly results in a controlled, wave-like release of histamine, a key triggering chemical involved in inflammation. But in the itchy rash of chronic hives, histamine release appears to be more spontaneous, suggesting that the histamine-carrying mast cells and basophils are abnormal.
Saini next plans more studies on omalizumab's effects on IgE, and how it contributes to chronic hives and rash. He says his goal is to understand the underlying mechanism of the disease and explain why the drug is effective.