Holistic scoring system of obesity treatment outcomes
A new scoring system takes a holistic view of the effect of obesity treatment in patients.
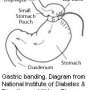
Bariatric surgery is the most successful treatment for obesity. Until now, the measure of treatment success has been limited to weight loss and remission of type 2 diabetes mellitus (T2DM) without any reference to the improvement in overall health in the individual patient.
As obesity becomes an ever-more prevalent condition in society today, its impact is evident on many aspects of the wellbeing and health of patients.
A team of researchers led by Conway Fellow, Professor Carel le Roux developed a system to assess nine aspects of the medical, psychological and functional state of a patient after bariatric surgery.
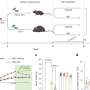
Each aspect is measured in four stages from normal health (stage 0) to advanced disease (stage 3) using quantifiable measures where possible or well-defined categories for qualitative measures.
The team used the new King's Obesity Staging system and its modified version to assess a group of 71 Northern Irish patients at the Royal Victoria Hospital in Belfast prior to, and one year after, bariatric surgery at Imperial College Healthcare NHS Trust in London.
They found significantly improved outcomes for patients one year after bariatric surgery with fewer patients in the more severe stages of every category. Patients with type 2 diabetes had similar outcomes to non-diabetic patients.
Not only does this system provide a way to evaluate the effect of obesity interventions in a holistic patient-centred way, it improves on the current scoring system, the Edmonton Obesity Scale, as it is less like to be affected by bias on the part of the assessor.
Speaking at the 2013 British Obesity and Metabolic Surgery Society meeting in Glasgow, Scotland, PhD student, Karl Neff said that the new system is designed to highlight all the benefits bariatric surgery can give to the patient rather than just the physical measurements normally relied on today.