Henry Ford Hospital pioneers new cardiac approach
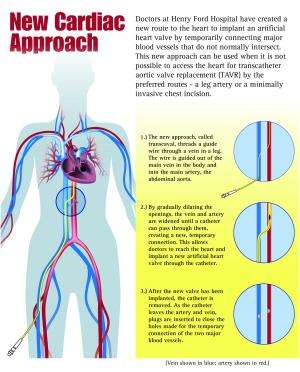
Doctors at Henry Ford Hospital have created a new route to the heart to implant an artificial heart valve by temporarily connecting major blood vessels that do not normally intersect.
In a July 3 operation on 79-year-old Viola Waller of Charlevoix, physicians performed a world-first cardiac procedure when it became evident that other means would not work.
"I knew of an experimental technique that had not yet been done in humans, and I had a patient with no other options who was failing rapidly," says William O'Neill, M.D., medical director of the Center for Structural Heart Disease at Henry Ford Hospital.
The new approach, called transcaval, involves threading a guide wire through a vein in a leg, and passing it from the main vein in the body into the main artery, the abdominal aorta. Then, by gradual dilation, the openings of the vein and artery are widened to the point of allowing a catheter to connect them, continue to the heart, and implant the new artificial heart valve.
As the catheter is removed, plugs are inserted in the artery and the vein to close the holes made for the temporary connection of the two major blood vessels.
Approximately 5 million people in the U.S. are diagnosed with heart valve disease each year. With an aging population that is often too frail for open-heart surgery, more than 20,000 Americans die of the disease each year, according to the American Heart Association.
Dr. O'Neill estimates that this new procedure could help 25,000 – 50,000 patients a year in the U.S.
Waller was transferred from northern Michigan to Detroit by medical helicopter in critical condition. Her aortic valve, a previous implant done through open-heart surgery many years ago, was failing.
The preferred access for transcatheter aortic valve replacement (TAVR) is through the leg arteries. However, Ms. Waller's arteries were too small in diameter for the catheter due to prior plaque buildup and stents that had been previously placed in them. Cardiologists made an attempt to reach her heart through a minimally invasive chest incision, but fatty deposits near the patient's heart could not support the necessary structure for a catheter.
"Since all traditional options were not feasible our multi-specialty team felt the new technique could be the answer for this patient," says Adam Greenbaum, M.D., director of the Cardiac Catheterization Lab at Henry Ford Hospital and leader of the team. "She could not have open-heart surgery, and her condition was deteriorating daily."
Robert Lederman, M.D., an interventional cardiologist and senior investigator at the National Institutes of Health who developed the technique in pigs, came to Detroit to observe the procedure and share his insights.
Waller is making a remarkable recovery, and has returned to her home in northern Michigan.
"The success of this new procedure may open a new route for transcatheter valve replacement," adds Dr. O'Neill.

















