Replacing insulin through stem cell-derived pancreatic cells under the skin
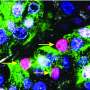
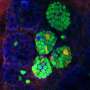
Sanford-Burnham Medical Research Institute and UC San Diego School of Medicine scientists have shown that by encapsulating immature pancreatic cells derived from human embryonic stem cells (hESC), and implanting them under the skin in animal models of diabetes, sufficient insulin is produced to maintain glucose levels without unwanted potential trade-offs of the technology. The research suggests that encapsulated hESC-derived insulin-producing cells hold great promise as an effective and safe cell-replacement therapy for insulin-dependent diabetes.
"Our study critically evaluates some of the potential pitfalls of using stem cells to treat insulin-dependent diabetes," said Pamela Itkin-Ansari, Ph.D., adjunct assistant professor in the Development, Aging, and Regenerative Program at Sanford-Burnham, with a joint appointment at UC San Diego.
"We have shown that encapsulated hESC-derived pancreatic cells are able to produce insulin in response to elevated glucose without an increase in the mass or their escape from the capsule. These results are important because it means that the encapsulated cells are both fully functional and retrievable," said Itkin-Ansari.
In the study, published online in Stem Cell Research, Itkin-Ansari and her team used bioluminescent imaging to see if encapsulated cells stay in the capsule after implantation.
Previous attempts to replace insulin-producing cells, called beta cells, have met with significant challenges. For example, researchers have tried treating diabetics with mature beta cells, but because mature cells are fragile and scarce, the method is fraught with problems. Moreover, since the cells come from organ donors, they may be recognized as foreign by the recipient's immune system—requiring patients to take immunosuppressive drugs to prevent their immune system from attacking the donor's cells, ultimately leaving patients vulnerable to infections, tumors, and other adverse events.
Encapsulation technology was developed to protect donor cells from exposure to the immune system—and has proven extremely successful in preclinical studies.
Itkin-Ansari and her research team previously made an important contribution to the encapsulation approach by showing that pancreatic islet progenitor cells are an optimal cell type for encapsulation. They found that progenitor cells were more robust than mature beta cells to encapsulate, and while encapsulated, they matured into insulin-producing cells, which secreted insulin only when needed.
"We were thrilled to see that the cells remained fully encapsulated for up to 150 days, the longest period tested, said Itkin-Ansari. "Equally important is that we show that the progenitor cells develop glucose responsiveness without a significant change in mass—meaning they don't outgrow their capsule.
"Next steps for the development of the approach will be to figure out the size of the capsule required to house the number of progenitor beta cells needed to respond to glucose in humans. And of course we want to learn how long a capsule will function once implanted. Given these goals and continued successful results, I expect to see the technology become a treatment option for patients with insulin-dependent diabetes," said Itkin-Ansari.