Statins may lower blood clot risk following joint replacement surgery
Statins have long been known to lower cholesterol and, more recently, to decrease the risk of deep vein thrombosis (blood clots) in healthy, non-surgical patients. New, first-of-its-kind research presented today at the 2014 Annual Meeting of the American Academy of Orthopaedic Surgeons (AAOS), found that statins, when used in conjunction with conventional blood clot prevention therapies, significantly reduced the risk for venous thromboembolic (VTE) events following total joint replacement (TJR) surgery.
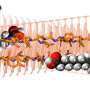
The number of total hip and total knee replacement surgeries continues to rise each year (more than one million were performed in 2011). And while these procedures are safe and effective, and diminish pain and restore mobility in the vast majority of patients, there is a risk for side effects, including the rare formation of a VTE ─ a blood clot located within a deep vein in the thigh or calf following surgery.
Current, standard VTE prevention techniques include the use of an elastic stocking and/or other external compression device upon admittance to the hospital, patient movement and rehabilitation beginning the first day after surgery and continuing for several months, and anticoagulant therapy (blood thinning medications) starting the night before surgery and continuing after the patient is discharged.
In this new study, researchers reviewed the outcomes of 546 total hip and knee replacement patients with a minimum of 11 months post-operative follow up. All patients received the standard VTE post-operative therapy, based on AAOS guidelines. Patients who received a revision joint replacement surgery, a TJR following a fracture, patients with a history of blood clots, or patients taking hormone replacement therapy were excluded from the study.
The average patient age was 65.5 years old, and 61 percent of patients were obese with a Body Mass Index (BMI) of 33 kg/m². Patients were divided into two groups: 196 patients who took statins before, during and after surgery (perioperatively); and 221 patients who did not take statins.
The statin group had a significantly lower amount of VTE events (15 patients or 7.7 percent) compared to the non-statin group (32 patients or 14.5 percent).
"Our study found that statins, in addition to conventional venous thromboembolic pharmacologic therapy, significantly reduced the event of VTE in the post-operative period for patients undergoing elective total hip and knee replacements," said Philadelphia-based orthopaedic surgeon and lead study author Katharine T. Criner, MD. "The relative risk of VTE with use of statins was reduced by 48 percent. Statins not only have lipid-lowering effects, but anti-inflammatory effects that may account for their ability to decrease the development of VTE."