Doctor's specialty predicts feeding tube use
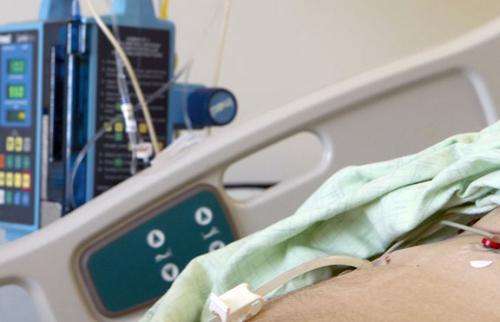
A new study shows that when elderly patients with advanced dementia are hospitalized, the specialties of the doctors at their bedside have a lot to do with whether the patient will end up with a gastric feeding tube – a practice that some medical organizations recommend against for frail, terminal patients.
In the April edition of the journal Health Affairs, researchers led by Brown University gerontologist Dr. Joan Teno found that in tens of thousands of cases over the last decade, patients were much less likely to receive a feeding tube when their attending physicians were primary care generalists or hospitalists than when at least some of their attending doctors were subspecialists. Patients with advanced dementia attended to by only hospitalists, for example, got gastric tubes only 1.6 percent of the time while patients with an attending mixture including subspecialists got them in 15.6 percent of cases.
Teno said the results can help explain why the practice of feeding tube insertion continues in patients with advanced dementia, even though it's rarely consistent with the family's desire for end-of-life care focused on providing comfort. Both The American Academy of Hospice and Palliative Medicine and the American Geriatrics Society recommend feeding advanced dementia patients by hand instead of via tubes.
"What we've done in the past is establish an evidence base that feeding tubes in this population are not effective, and we have documented tremendous variation in hospitals' insertion rates of feeding tubes," said Teno, a hospice physician who teaches in the Brown University School of Public Health. "Now we are trying to understand what's inside that black box of the hospital that explains why some people are more likely to have a feeding tube insertion."
A decade of data
To study the influence of physician specialty, Teno and her colleagues combined Medicare billing data with nursing home records to identify cases between 2001 and 2010 in which nursing home residents with dementia were hospitalized. From the records, the team could tell the specialty of the hospital attending physician each day of the hospital stay and whether the patients received a gastric feeding tube.
To minimize confounding medical complications in the data, Teno's team focused on hospital admissions stemming only from infections (such as pneumonia) or dehydration and excluded patients who visited the intensive care unit. Even so, more than 50,000 cases qualified for their analysis.
In their analysis, the researchers statistically controlled for the degree of patient dementia, their length of stay, and a variety of demographic, medical, and geographic factors.
The clear pattern, independent of these other factors, was that the two care scenarios that are increasingly common in hospitals—attending care entirely by hospitalists or attending care from mixed-specialty groups of physicians—were polar opposites in terms of feeding tube insertion frequency.
"It's very stark," Teno said. "We are making fairly striking changes in who cares for these patients in the acute care hospital. In the past decade, we're seeing a lot of changes in who the attending type is even during a brief hospital stay."
Meanwhile, the study found that patients became less likely over the decade for their attending physicians to be either all non-hospitalist generalists (who inserted feeding tubes 2.2 percent of the time) or all sub-specialists (who inserted tubes 11 percent of the time).
What to do
The persistence of feeding tube insertion among sub-specialists may be a gap in their continuing medical education, Teno said, or it may come from being too focused on a narrow aspect of a patient's condition.
"A lot of what we're seeing here is specialists who tend to focus on body organs and not a holistic approach to patients," Teno said. "You need a holistic picture when you think about this patient population. It's really the extent of cognitive impairment that should guide decision making."
One solution is to ensure that a patient's parade of attending physicians is marching in step.
"Hospitals should ensure coordination of care when patient handoffs are made between different types of attending physicians," the authors wrote in Health Affairs.
But Teno said the best solution is almost certainly to reduce such hospitalizations in the first place. Nursing home residents with advanced dementia are often harmed rather than hurt by such burdensome transitions between facilities. Infections can often be treated as effectively in the nursing home as in the hospital, she said.