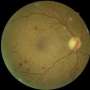
Plugging leaky blood vessels to save vision
A new drug approach has been developed for safer clean-up of deformed blood vessels in the eye by a research team at the Lunenfeld-Tanenbaum Research Institute, Mount Sinai Hospital in Toronto.
The growth of malformed blood vessels that can burst is a leading cause of vision loss in North America. Retinopathy and retina degeneration are associated with premature birth, with diabetes, and with increasing age.
Research just published by Dr. Andras Nagy and co-authors shows both safety and effectiveness in their bioengineered compound when treating retinopathy in mice. The therapeutic, which they called "Sticky-trap," shuts down tiny deformed blood vessels in the eye without affecting healthy vessels in other sites of the body.
The research appears in EMBO Molecular Medicine, which published a separate editorial stating that the compound "holds great promise as a strategy that could be rapidly translated into clinical practice. […] We expect that Sticky-trap and future related molecules will have significant impact on the field of tumour biology in local control of recurrent disease. […]"
Dr. Nagy is a Senior Investigator at the Lunenfeld-Tanenbaum and holds a Canada Research Chair in Stem Cells and Regeneration. He is a Professor in the Department of Obstetrics and Gynacology at University of Toronto and an Investigator at the McEwen Centre for Regenerative Medicine. Co-authors include colleagues from University of California Los Angeles, The Scripps Research Institute (La Jolla CA), University of Toronto, and the Lunenfeld-Tanenbaum.
Selective action is key to safety
Like some other treatments for retinopathy, Sticky-trap is injected into the eye. The potential game-changer is Sticky-trap's safety profile. It is stable and long-lasting once in the eye. If the compound gets into the circulation, it quickly inactivates – ensuring that it does not affect other blood vessels, tissues, and organs.
A problem in this research arena – called antiangiogenesis – has been finding a compound that is selective, closing off abnormal blood vessels only in the diseased organ while leaving all others intact. "That's difficult, and it's what makes this research high-risk as well as high-impact," Dr. Nagy says.
Type 2 diabetes illustrates the challenge. "Patients with diabetic retinopathy are losing vision because blood vessels in their eyes overgrow, become deformed and burst, often tearing the retina in the process. Drugs that suppress the excess vessel formation in the eye could negatively affect healthy organs if they escape into the blood, causing kidney function problems, poor wound healing, and hypertension," Dr. Nagy adds. These side effects are serious health threats that the Sticky-trap approach can avoid.
Advanced bioengineering
Over the nine years it took to bring the project to fruition, Dr. Nagy's team used cutting-edge genetic and pharmacological techniques to engineer the new two-step biologics. Sticky-trap includes a binding component that attaches to the surface of cells, ensuring that it remains in place and is stable, as well as the biologically active component. "That's important when a treatment involves injection directly into a diseased tissue," says first author Dr. Iacovos Michael, a post-doctoral fellow in the Nagy lab. "The longer-acting it is, the fewer injections a patient will need." He adds that the project "is just the beginning for the establishment of a new class of pharmacological entity, 'sticky' biologics, characterized by localized, targeted activity. The same principle could be used to develop similar local-acting biologics for other conditions such as inflammatory and autoimmune diseases."
Dr. Nagy is renowned for his work in stem cells, blood vessel biology, and creating genetic tools in cancer cells, among other areas. His team is also working on applications of the two step Sticky-trap for solid tumours.
Upon publication on May 6, Sticky-trap became available to biotech and pharmaceutical companies to adapt and develop.
"The significant advance in this approach is its built-in precision guidance system," says Dr. Jim Woodgett, Director of the Lunenfeld-Tanenbaum. "Worldwide research efforts have developed powerful agents that can treat diseased tissues but if they cannot be steered to where they are needed, they can also cause collateral damage. The initial application to diabetic retinopathy shows proof-of-principle in a very important disease, but the approach can be adapted to other powerful drugs and diseases where localized activity is needed."
More information: The research paper is "Local acting Sticky-trap inhibits vascular endothelial growth factor dependent pathological angiogenesis in the eye," on-line May 6 2014 in EMBO Molecular Medicine.