Addressing the physician shortage: Recommendations for medical education reform
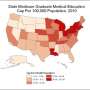
Since it started more than 30 years ago, funding the graduate medical education (GME) system has not evolved even as there has been a revolution in GME. The United States contributes almost $10 billion a year from Medicare into funding the GME system. However this system fails to provide the workforce needed for the 21st century and lacks the necessary transparency and accountability.
With an aging population and millions of people newly registered for health insurance because of the Affordable Care Act, there is a pressing need to increase the number of primary care physicians. In the United States, it is estimated that only 20.9 percent of residents graduating from GME programs will practice primary care.
Recommendations recently published in the Journal of General Internal Medicine prepared by the Health Policy Education Subcommittee of the Society of General Internal Medicine (SGIM) outline how to reform the GME system to support the development of a physician workforce that can provide high quality, high value, population-based, and patient-centered health care, aligned with the dynamic needs of America's healthcare delivery system.
Angela Jackson, MD, associate dean for student affairs at Boston University School of Medicine and a physician in general internal medicine at Boston Medical Center, is the article's first author and is Co-Chair of the SGIM's Health Policy Committee.
"SGIM hopes its policy and paper will invigorate the debate on GME funding, moving beyond discussions limited to funding levels to discussions on GME program accountability for public fund use and how to shape a GME system that will provide the nation with the physician workforce that we need," said the authors.
The recommendations address workforce analysis, funding mechanisms, transparency, competency-based curriculum accountability, distributions of physician specialties and educational innovation, and call for:
- Fully funding the National Health Care Workforce Commission
- Having all payers for care contribute toward GME
- Rebasing direct and indirect medical education payments to reflect 21st century costs
- Requiring transparency in spending GME funds
- Using GME funding exclusively for trainee education and related costs
- Requiring training programs demonstrate their graduates are competent to practice 21st century medicine
- Developing incentives for training programs to align the practice patterns of their graduates with regional and national workforce needs
- Funding to develop GME innovations designed to impact the physician workforce positively.