Study examines effect of adding insulin with metformin to treat diabetes
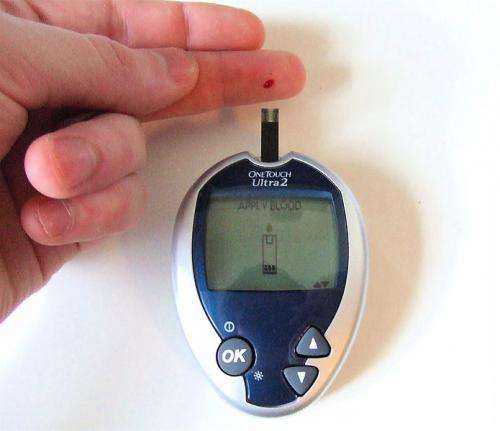
Among patients with diabetes who were receiving metformin, the addition of insulin compared with a sulfonylurea (a class of antidiabetic drugs) was associated with an increased risk of nonfatal cardiovascular outcomes and all-cause death, according to a study in the June 11 issue of JAMA, a diabetes theme issue.
Diabetes mellitus and its complications represent an enormous health care burden and result in nearly 200,000 deaths annually. The American Diabetes Association and the European Association for the Study of Diabetes recommend that, for patients with preserved kidney function, diabetes treatment begin with metformin and lifestyle changes to achieve a glycated hemoglobin (HbAlc) level of less than or equal to 7 percent. Often patients will require a second agent to reach this goal, but there is no consensus regarding which medication to choose, according to background information in the study.
Clinicians begin administration of insulin to attain fast and flexible control of blood glucose levels. Because of the promising results of a few trials, there has been an increase in early initiation of insulin and its use as add-on therapy to metformin.
Christianne L. Roumie, M.D., M.P.H., of the Veterans Health Administration-Tennessee Valley Healthcare System Geriatric Research Education Clinical Center, and Vanderbilt University, Nashville, Tenn., and colleagues conducted a study with data from national Veterans Health Administration, Medicare, and National Death Index databases, which included veterans with diabetes initially treated with metformin from 2001 through 2008 who subsequently added either insulin or sulfonylurea. The researchers compared the risk between therapies of a composite outcome of heart attack, stroke, or all-cause death.
Among 178,341 metformin monotherapy patients, 2,948 added insulin and 39,990 added a sulfonylurea. The authors performed additional propensity matched analysis on a subset of 2,436 patients from the insulin group and 12,180 patients from the sulfonylurea group. Patients had received metformin for a median of 14 months before adding another therapy; median follow-up after this addition was 14 months. An analysis of the subsequent events indicated that heart attack and stroke rates were statistically similar, whereas there was a higher rate of all-cause death among patients who received insulin.
"Our finding of a modestly increased risk of a composite of cardiovascular events and death in metformin users who add insulin compared with sulfonylurea is consistent with the available clinical trial and observational data. None of these studies found an advantage of insulin compared with oral agents for cardiovascular risk, and several reported increased cardiovascular risk or weight gain and hypoglycemic episodes, which could result in poorer outcomes," the authors write. "Our study suggests that intensification of metformin with insulin among patients who could add a sulfonylurea offers no advantage in regard to risk of cardiovascular events and is associated with some risk."
"These findings require further investigation to understand risks associated with insulin use in these patients and call into question recommendations that insulin is equivalent to sulfonylureas for patients who may be able to receive an oral agent."
In an accompanying editorial, Monika M. Safford, M.D., of the University of Alabama at Birmingham, comments on comparative effectiveness research, such as the study conducted by Roumie and colleagues.
"Comparative effectiveness research is creating new challenges as it generates much needed new evidence. The very methods that make studies like that of Roumie et al novel also create barriers to interpretation that may make it more difficult to apply their results. Some of the creativity being brought to bear on advancing methods of analysis may also be needed to advance methods of communicating both methods and results to practicing clinicians, and perhaps more importantly, to the patients who are facing decisions that may (or may not) have profound implications for their health and well-being."
More information:
DOI: 10.1001/jama.2014.4312
DOI: 10.1001/jama.2014.4313