Scientists identify drivers of rheumatoid arthritis
Researchers at Benaroya Research Institute at Virginia Mason (BRI) used cutting-edge tetramer technology developed at BRI to find the T cells that drive rheumatoid arthritis (RA). "By using tetramer technology, we were able to examine whether T cells in people with rheumatoid arthritis were increased in number or were unique in other ways," says BRI Associate Director Jane Buckner, MD, who led the study with BRI Tetramer Core Laboratory Manager Eddie James, PhD. The findings were recently reported online in Arthritis & Rheumatology.
This tool now allows scientists to study how RA starts, how current therapies may impact the immune response directed to the joint and how to specifically target these cells therapeutically. "For the first time, we were able to demonstrate that T cells that recognize proteins in the joint were increased in the blood of people with RA and that these cells had a unique set of markers. Further we were able to demonstrate that the number of these cells changes over time in patients and with treatment." BRI is an international leader in developing tetramer technology which allows scientists to isolate cells that are difficult to pinpoint, often compared to finding a needle in a haystack.
"RA is a debilitating disease affecting people of all ages including children," says Dr. Buckner. "Many people are diagnosed in their early 20's, 30's and 40's, and it impacts them at a very productive time of their lives. We used to see people with RA in wheelchairs and needing joint replacements, but during the last 15 years we have seen incredible progress in new therapies. If people are appropriately diagnosed and treated, they can work full time and be healthy, active adults. But they can still suffer and need medications that have risks and side effects. The drugs can be costly and sometimes they don't work or eventually stop working. If untreated, the disease will permanently destroy joints and cause pain. We would like to find ways to treat people early and target only the cells that cause the disease and eventually, prevent this disease."
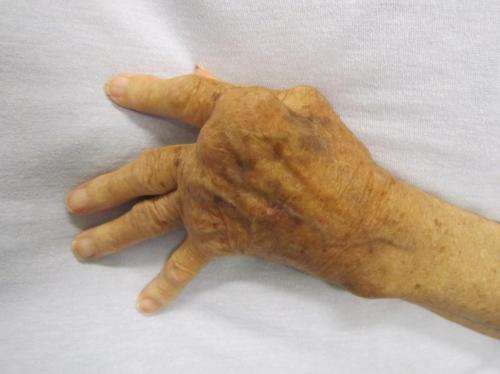
Rheumatoid arthritis is thought to be a T cell mediated disease and is caused when the body's immune system mistakenly begins to attack its own tissues, primarily the synovium, the membrane that lines the joints. As a result of this autoimmune response, fluid builds up in the joints, causing joint pain and systemic inflammation.
RA is a chronic disease in which most people experience intermittent periods of intense disease activity punctuated by periods of reduced symptoms or even remission. In the long term, RA can cause damage to cartilage, tendons, ligaments and bones which can lead to substantial loss of mobility.
An estimated 1.3 million people in the United States have RA—almost 1 percent of the nation's adult population. There are nearly three times as many women as men with the disease. In women, RA most commonly begins between the ages of 30 and 60. In addition, as many as 300,000 children are diagnosed with a distinct but related form of inflammatory arthritis called juvenile arthritis.
This work was funded by an Autoimmune Disease Prevention grant from the National Institutes of Health. A new grant of $1.3 million from the U.S. Department of Defense will extend the discovery to ask in-depth questions about whether these T cells reflect disease activity and if they change in patients who respond to therapy. Drs. Buckner and James will lead the study with Bernard Ng, MD, Chief of Rheumatology, Veterans Affairs Puget Sound Healthcare System. Research will include biorepository studies of samples voluntarily provided by Veterans Affairs and BRI research participants who help to advance science.