Protein on 'speed' linked to ADHD
A genetic change in the dopamine transporter – one of the brain's dopamine-handling proteins – makes it behave as if amphetamine is present and "run backward," Vanderbilt University Medical Center investigators report this week in The Journal of Neuroscience.
The altered function of the transporter gene variant, discovered in two brothers with attention deficit hyperactivity disorder (ADHD), supports a role for dopamine signaling in the disease. ADHD is one of the most common mental health disorders in children and adolescents, affecting up to 5 percent of school-age children in the United States.
"We believe that this is important evidence that ADHD can be caused by a functional deficit in the brain's dopamine signaling pathway," said Randy Blakely, Ph.D., director of the Center for Molecular Neuroscience.
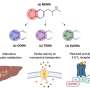
The researchers propose that because the altered transporter runs backward and pushes dopamine out into the space between neurons – like normal transporters do when amphetamine, or 'speed,' is present – it alters dopamine signaling and contributes to the symptoms of ADHD.
"It's like these kids are on amphetamine all the time," said Aurelio Galli, Ph.D., an investigator in the center. Amphetamine causes hyperactivity, paranoia and psychosis in normal subjects.
Variations in brain dopamine signaling have long been suspected to participate in the development ADHD and other neuropsychiatric disorders. Dopamine has roles in brain circuits linked to attention, motor function, reward and cognition, and drugs that target dopamine transporters and receptors are used to treat ADHD, bipolar disorder and schizophrenia.
Because the dopamine transporter is a key member of the dopamine-signaling network, Blakely and colleagues searched for changes in this protein in patients with ADHD. They found a single "letter" change in the transporter gene in two brothers. The particular mutation had been reported once before in a patient with bipolar disorder, which also has connections to dopamine signaling, but the functional impact of the mutation had not been pursued, Blakely said.
In initial studies of the variant transporter in cultured cells, the group found no differences in function compared to the normal transporter – the mutant transporter moved dopamine into the cell and was appropriately regulated by dopamine transporter blockers and cellular signaling pathways.
Turning to a sensitive technology called amperometry that uses a small carbon fiber to "listen in" on how single cells release or transport dopamine, the Galli and Blakely laboratories discovered that the altered transporters were running backward at an exaggerated rate, literally pushing dopamine out of the cell.
"We think this activity would short circuit the normal synaptic transmission process," Blakely said. "Instead of the precise 'pop-pop-pop' of dopamine being released from vesicles (tiny packets of neurotransmitter), there's a cloud of dopamine bleeding out, and the dopamine signaling system is not as sharp as it should be."
To their surprise, the investigators also found that amphetamine blocks the leak of dopamine through variant transporter. Normally, amphetamine does just what the mutation does – it causes the dopamine transporter to run in the reverse direction.
The findings offer a new perspective on a conundrum in the ADHD field – the fact that two of the medications that successfully treat the disease have opposing effects on their molecular target, the dopamine transporter. With the normal dopamine transporter, methylphenidate (Ritalin) blocks the ability of amphetamine (Adderall) to make the transporter run backward, yet both drugs are equally beneficial to patients with ADHD.
But when the transporter runs backward of its own accord – as it does with this rare mutant version – both agents act as blockers and stop the leak of dopamine.
"This observation unifies the action of these drugs and strongly suggests that backward-running transporters may be an important mechanism in ADHD, even for those who do not have this particular mutation," Blakely said.
Researchers studying the dopamine transporter have found that there are multiple ways to cause the transporter to run backward, Galli pointed out, and the team is now screening other genes in the "network of signaling pathways that target the transporter and reverse dopamine flow" as potential contributors to ADHD risk.
The investigators also speculate that backward-running transporters may represent a more general phenomenon, giving rise to multiple types of neuropsychiatric disorders.
"Millions of patients have taken drugs that block transporter proteins, such as those that handle brain norepinephrine and serotonin, to treat anxiety and depression," Blakely said. "We used to think that the only thing these drugs could do is block uptake – now we wonder if reducing the backward leak of neurotransmitter is a key component of their utility."
Source: Vanderbilt University