Blood vessel cells are instructed to form tube-like structures
How do blood vessel cells understand that they should organise themselves in tubes and not in layers? A research group from Uppsala University shows for the first time that a special type of "instructor" molecule is needed to accomplish this. These findings, published in the scientific journal Blood, might be an important step towards using stem cells to build new organs.
In order for a body to develop and function the cells in the body must be able to organise themselves in relation to each other. The way in which cells are arranged depends on the organ where they are located. Blood vessel cells need to form three-dimensional, tube-like structures that can transport blood. But how do blood vessel cells know that they should do that? An important part of the communication between cells and their environment is the use of growth factors. These are proteins that bind to receptors on the surface of the cell that receives the information. When the receptor in turn forms a complex with other proteins, on the inside of the cell, the read-out from the DNA can be altered. The information has "arrived".
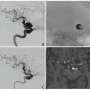
VEGF (vascular endothelial growth factor) is a family of closely related growth factors that control blood vessel cells throughout life. Blood vessel development in the foetus as well as later in life, for example during wound healing, is regulated by VEGF. In the present study the research group has examined how VEGF can instruct blood vessel cells to arrange themselves into a tube. The answer is that some variants of VEGF have the ability to attract another protein, an instructor molecule, which is joined together with VEGF and its reeptor. The combination of instructor molecule, VEGF and receptor results in that a specific signal is sent inside the blood vessel cells, making them form a tube. Without the instructor molecule the cells line up next to each other, in a layer.
These results may become very useful. Today stem cells are used to create new cells, organs and even tissues, that in the future might be used to for transplantation instead of donated organs. If a patient's own stem cells are used the problem with organ rejection is avoided. But so far there has been a challenge to create three-dimensional structures from stem cells.
Our contribution can make it possible to create blood vessels from stem cells and to direct them to form a tube instead of a layer. Perhaps this knowledge can be transferred to the formation of other tube-like structures in the body, such as the lung and intestines. The perspectives for the future are very exciting, says Lena Claesson-Welsh, who has led the study.
Source: Uppsala University