Eroded telomeres are behind a rare premature aging syndrome
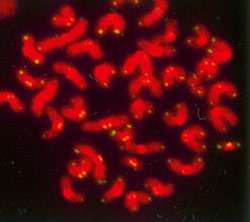
(PhysOrg.com) -- Each time a cell divides, the protective caps at the ends of chromosomes shorten — and when these caps are gone, so are we. Now, by using an unconventional strategy to shorten telomeres in mice, researchers at Rockefeller University have not only created the first faithful mouse model for studying a rare yet fatal premature aging syndrome, but they have revealed the molecular defect behind the disease.
At a time when the world seems to be age-obsessed, this research may ultimately help scientists disentangle which genes play a role in the normal aging process from those involved in age-related disease.
“Our mouse model is a step forward in understanding the pathogenesis of this disease and it may help us understand how we age in general,” says Titia de Lange, head of the Laboratory of Cell Biology and Genetics and Leon Hess Professor at Rockefeller University.
Sufferers of the disease, called dyskeratosis congentia, tend to have problems in tissues in which cells multiply rapidly — skin, hair, nails, tongue, gut and bone marrow — and usually die between the ages of 16 and 50 from bone marrow failure, or the inability to replenish their blood cells. According to some estimates, dyskeratosis congenita has only been diagnosed in 70 individuals since it was first described in 1906. “But the disease is probably much more frequent than previously inferred,” says de Lange, “as it is part of a spectrum of disorders with diverse clinical manifestations, such as anemia and lung fibrosis.”
Although patients were found to have severely shortened telomeres at the time of diagnosis, perplexing findings emerged that left researchers wondering whether dyskeratosis congenita was a telomere-based disease after all. When bits of DNA are lost from telomeres during each cell division, telomeres are partially rebuilt with an enzyme called telomerase. However, when researchers genetically engineered mice that didn’t produce telomerase, the mice had very short telomeres but didn’t show any signs of the disease, particularly its hallmark: bone marrow failure.
De Lange and her former graduate student Dirk Hockemeyer, who graduated in 2007, took a different approach: They made mice that lack POT1b, a protein that protects telomeres from getting degraded. Without POT1b, mice do not show the signs and symptoms of dyskeratosis congenita, but the telomeres shorten so fast that telomerase is incapable of keeping up with the loss. But without POT1b and reduced telomerase activity, mice develop the major hallmarks of the disease and die of bone marrow failure. When the mice that lacked POT1b were bred with mice that lacked telomerase, the offspring died.
“Dirk’s mutant mouse is the first faithful mouse model for a human telomere disease” says de Lange. “Together, these results suggest that in patients suffering from dyskeratosis congenita, the enzyme telomerase can’t elongate telomeres as fast as the nucleases chew them away.”
“Clearly, the next step is to understand how telomeres are degraded in human cells,” says de Lange. “We need to identify the nucleases at work and find out how they are regulated — a problem that will have to be tackled by a next generation of graduate students.”
Citation: Genes & Development 22: 1773–1785 (June 2008)
Provided by Rockefeller University