Childhood wheezing with rhinovirus can increase asthma odds 10-fold
Infants who experience viral respiratory illnesses with wheezing are known to be at increased risk for developing asthma later during childhood. It is not known, however, whether every type of respiratory virus that produces wheezing presents similar risk. Using new molecular techniques to identify different viruses, researchers now believe they have pinpointed the biggest culprit: rhinovirus (RV).
"We have found that rhinovirus, the most common cause of colds, contributes a disproportionate amount towards future asthma development in comparison to other viruses that also cause childhood wheezing," said principle investigator, Robert F. Lemanske, Jr., M.D., head of the Division of Pediatric Allergy, Immunology, and Rheumatology and Professor of Pediatrics and Medicine at the University of Wisconsin School of Medicine and Public Health.
The results were reported in the first issue for October of the American Journal of Respiratory and Critical Care Medicine, published by the American Thoracic Society.
From November 1998 to May 2000, researchers at the University of Wisconsin recruited nearly 300 newborns at high risk for asthma (with one or both parents having had allergies or asthma) to take part in their prospective cohort study on the etiology of asthma, the Childhood Origins of Asthma (COAST) study. The children were followed from birth to six years and evaluated for the presence of specific viruses during wheezing illnesses.
At six years, 28 percent of the kids had asthma— and those who had wheezed with rhinovirus were disproportionately among them. Children who wheezed with RV during the first year of life were nearly three times as likely to have asthma at age six, whereas children who wheezed with respiratory syncytial virus (RSV), another common respiratory ailment that has been linked to asthma risk in children, did not have an increased asthma risk.
The older the children were, the greater the effect. Children who had wheezed with RV in their second year of life were more than six times as likely to have asthma. Wheezing with RV at three increased asthma odds by more than 30-fold.
The study confirmed previous findings that wheezing with RSV any time during the first three years led to a nearly three-fold increased asthma risk. However, the novel finding is that "wheezing RV illnesses occurring at any time during the first three years of life were associated with a nearly 10-fold increase in asthma risk at six years, making them the most significant predictor of asthma development in the high risk COAST cohort," wrote Daniel J. Jackson, M.D., Allergy and Immunology Fellow at the University of Wisconsin, lead author of the article.
"Indeed, nearly 90% of the children wheezing with RV during year three subsequently developed asthma at age six," he wrote.
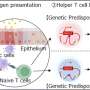
Whether RV causes asthma to develop, or simply reveals children who are already predisposed to the disease (host-related factors) remains an open question. Alternatively, "In genetically susceptible children, RV wheezing illnesses could cause airway damage as well as subsequent asthma (virus-related factors)," stated Dr. Jackson, pointing out that the possibilities are not mutually exclusive and that additional research would be required to resolve the question.
These findings mark a shift in medical knowledge on the topic of virus-induced wheezing and subsequent asthma development. John E. Heffner, M.D., past president of the ATS, stated that "the results of this study represent important advances in our understanding of childhood asthma because the investigators studied infants in an outpatient setting. Prior studies examined more seriously ill, hospitalized infants— mild viral illnesses may be just as important for later asthma as more severe infections. Also, the elegant technique used to identify specific viruses provides a foothold for understanding the unique viral attributes that cause wheezing and— potentially— lead to asthma."
Source: American Thoracic Society