Antibiotic Use Boosts Risk of Infection with Clostridium Bacteria
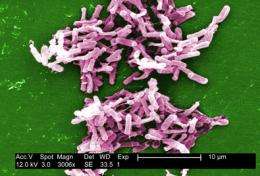
Antibiotic-resistant Staph infection is not the only emerging bacterial threat. Now a different bug — Clostridium difficile - is gaining strength.
C. difficile causes mild or severe diarrhea and, while rare, in some cases gets into the bloodstream, where it is life threatening. In the past C. difficile was largely limited to nursing home and hospital patients. But as with the better known MRSA bacteria responsible for many Staph infections, C. difficile cases increasingly are being reported among people who generally are healthy - especially among those who have taken antibiotics recently.
Infection can spread as a result of fecal contamination. The bacterium produces long-lived spores that can survive a long time outside the body - making it especially important to clean up around afflicted patients.
But poor infection control is not always the cause, notes Joseph Guglielmo, PharmD, chair of clinical pharmacy for the UCSF School of Pharmacy, and a research expert on antibiotic use in medicine. In most people a small amount of C. difficile can be present in the gut, he explains. But use of certain antibiotics can kill the bacterial competition and allow the C. difficile population to explode.
“Antibiotics, whether used appropriately or inappropriately, are absolutely a risk factor,” Guglielmo says.
“Hypervirulent” C. difficile
Furthermore, a new strain is on the loose. C. difficile makes a toxin that destroys the lining of the colon, and the new strain produces 20 to 30 times as much of this toxin as older strains, Guglielmo says. The new, “hypervirulent” strain is much more likely to be associated with more severe disease, sometimes requiring surgical intervention. Both the normal strains and the hypervirulent strain are becoming more common on the East Coast and in Canada, Guglielmo says.
While he was conducting rounds as an attending hospital pharmacist recently, Guglielmo encountered a patient who had been receiving chemotherapy as an outpatient and who had just been admitted to the hospital with diarrhea originally thought to be due to the chemotherapy. Despite a relatively normal abdominal exam, the patient had a high white blood cell count, suggesting a serious infection. The patient was treated immediately, without waiting for results of tests to detect C. difficile infection. He died the next day, before the positive test results came back.
Physicians may have to wait up to three days for results of the diagnostic test, according to Steve Miller, MD, PhD, director of the clinical microbiology lab for UCSF Medical Center. UCSF will soon begin using a test that does not rely on cell culture - one which will yield results in hours. However, this test and no other clinical diagnostic test approved by the US Food and Drug Administration can be used to distinguish normal and hypervirulent forms of C. difficile, Miller says. It’s not certain that the patient Guglielmo saw was infected with the hypervirulent strain.
If an outbreak of the hypervirulent form was suspected, it would be possible to send samples to state public health laboratories or to the US Centers for Disease Control and Prevention for testing, but it could take 10 days for results, Miller says.
Despite the trends elsewhere, C. difficile infection rates for UCSF hospital patients have remained stable over the past few years - in part due to an infection-control and hand-washing campaign, Miller says. “It’s definitely the number one cause of hospital-acquired diarrhea,” he says. “A large number of patients are on antibiotics, so you do expect a fair number of cases.” But as for the hypervirulent strain, he adds, “I haven’t seen any evidence that we’re seeing a lot of it here over the last few years.”
Antibiotics that Pose Infection Risk Differ Among Bacterial Strains
With C. difficile, antibiotics are a double-edged sword. Some antibiotics increase risk of infection. But when C. difficile infection already has taken hold, other antibiotics are needed to combat it.
A standard treatment for milder infections is metronidazole taken in pill form. More serious infections, including those triggered by the hypervirulent strain, require more aggressive treatment, Guglielmo says. Research has confirmed that the antibiotic of choice for potentially life-threatening infections should now be vancomysin, also taken orally, he says. Vancomycin concentrates in the gut, ground zero for C. difficile infection. Oral metronidazole acts in the gut, too, but it also is systemically absorbed into the bloodstream.
“For severe infection, the treatment is the same, but the outcomes are far more problematic with the hypervirulent strain,” Guglielmo says.
The antibiotics thought to increase risk for hypervirulent C. difficile are different from those earlier shown to increase risk for infection with normal strains.
“With the older strains of C. difficile, clindamycin and beta-lactam antibiotics such as penicillin and the cephalosporins were the ones associated with C. difficile infection,” Guglielmo says.
A different class of antibiotics called fluoroquinolones, the best known of which is ciprofloxacin, appears to foster infection with the hypervirulent strain of C. difficile.
“While it’s not proven yet, there is a concern that the broad use of fluoroquinolones in the community is a risk factor for this hypervirulent form,” Guglielmo says.














