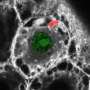
'Needle-free' intervention as natural vaccine against malaria
A study published in the journal Science Translational Medicine proposes that preventative treatment with affordable and safe antibiotics in people living in areas with intense malaria transmission has the potential to act as a 'needle-free' natural vaccine against malaria and may likely provide an additional valuable tool for controlling and/or eliminating malaria in resource-poor settings.
The research, conducted by a multinational team of researchers from the London School of Tropical Medicine and Hygiene (LSHTM), Heidelberg University School of Medicine, the Max Planck Institute for Infection Biology, Germany, and the KEMRI-Wellcome Trust Research Programme, Kenya, found that infection with malaria parasites during administration of preventative antibiotics developed a vaccine-like immunity against re-infection.
Approximately half the world's population is at risk of malaria and about one million people (mainly children living in sub-Saharan Africa) die each year from malaria, a mosquito-borne parasitic disease. Malaria parasites are transmitted to people through the bite of an infected Anopheles mosquito. Only an estimated 10 to 100 parasites per mosquito bite invade the liver where they replicate. About a week after infection, tens of thousands of parasites are released into the bloodstream where they are responsible for malaria's recurring fevers and cause life-threatening complications.
In this study, the researchers showed that the antibiotics caused a cellular defect in malaria parasites during their passage into the liver of the infected host. This action did not prevent parasite replication in the liver but blocked the malaria parasite's fatal conversion to the disease causing blood stage. The very late arrest of parasites in the liver allowed the immune system to mount a robust defence against subsequent infections, akin to experimental whole organism vaccine strategies using attenuated parasites.
As already established, antibiotics, especially in combination with other anti-malarial drugs, are safe and affordable drugs against an acute malaria infection. The novel concept is to take advantage of the immunological benefit of antibiotic prophylaxis in areas of moderate to high malaria transmission. In these settings, humans are continuously exposed to new malaria infections delivered by natural mosquito transmission that can be prevented by antibiotics. In the liver, a surplus of parasites presented to the immune system results in robust induction of memory immune responses that can recognize and destroy future malaria infections in the liver, when antibiotics are no longer taken.
Dr Steffen Borrman co-author on the paper says that 'this proof-of-principle study attempts to bridge a gap between basic malaria research and a rapid translation to a potential application in malaria-endemic countries. An important follow-up of this work is the validation of our experimental approach by clinical trials in humans. If successful, periodic administration of antibiotics, preferably in drug combinations, in high-risk population groups, particularly young, non-immune children, may provide an additional valuable tool for controlling and/or eliminating malaria in resource-poor settings.'