Predicting fracture risk with new imaging technology
A new method for identifying which bones have a high risk of fracture, and for monitoring the effectiveness of new bone-strengthening drugs and techniques, has been developed by scientists at the University of Cambridge.
The method, developed by Dr. Graham Treece and Dr. Andrew Gee of the Department of Engineering and Dr Ken Poole of the Department of Medicine, uses CT imaging to accurately measure the thickness of the cortical bone - the hard outer layer of compact bone which surrounds the spongy trabecular bone. The thickness of cortical bone is a key indicator of the risk of fracture.
This work is expected to lead to advances in the treatment and management of osteoporosis, a condition that affects one in two women and one in five men over the age of 50 in the UK.
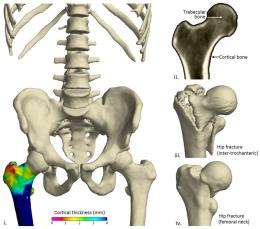
Osteoporosis results in a decline in bone strength and thinning of the cortical bone, so that often the remaining bone is no thicker than an eggshell by the time an individual is in their 80s. At certain key points, this thinning can lead to bones that are so weak that a stumble, trip or fall can lead to a fracture.
Currently, the key technology used to assess a patient's risk of fracture is a bone mineral density test, which uses dual-energy x-ray absorptiometry (DXA) to estimate mineral levels contained in bone. An alternative is multi-detector computed tomography (MDCT), which provides more comprehensive 3D imaging of bone structure, but not at a sufficient enough resolution to provide accurate sub-millimetre measurement.
The method developed by Drs Treece and Poole increases the accuracy of cortical bone measurements to the extent that clinicians can map changes in thickness over time, and produces accurate measurements of thicknesses as low as 0.3 mm.
Utilising data from a CT scan and a mathematical model of the scanning process, thousands of cortical bone measurements are obtained. This produces 3D thickness maps, which allows the identification of dangerously thin areas, Successive imaging allows maps to be produced depicting changes in the cortical bone over time in all areas of the skeleton so that the progress of osteoporosis treatments can be monitored.
"Osteoporosis is a condition which will become more and more common as the population ages," said Dr. Andrew Walsh of Cambridge Enterprise, the University's commercialisation group. "This exciting technology has the potential to improve the treatment of patients suffering from osteoporosis as well as to support the development of new drugs."
Dr. Poole presented this work at the Annual Meeting of the American Society for Bone and Mineral Research, held recently in Toronto. It will be further demonstrated at the annual meeting of the Radiological Society of North America, to be held in Chicago this November.
















