ATS issues report recommending research priorities in treatment of sleep apnea
The American Thoracic Society has released a new official report recommending research priorities in incorporating ambulatory management of adults with obstructive sleep apnea (OSA) into healthcare systems. The report identifies barriers preventing incorporation of portable monitor testing into clinical management pathways and recommends research and development needed to address those barriers.
The statement appears in the March 1, 2011, issue of the Proceedings of the American Thoracic Society.
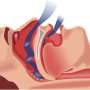
It is estimated that OSA occurs in roughly 20 million Americans, and occurs when the upper airway becomes constricted during sleep, blocking normal airflow and causing breathing to stop temporarily. Obesity is the greatest risk factor for OSA, but the disorder can occur in people who are not overweight. OSA is now widely recognized as a major public health concern and studies have linked OSA with increased risk of cardiovascular disease and motor vehicle accidents. OSA is diagnosed using polysomnography (PSG), a technique that measures a patient's breathing and oxygen level during sleep. PSG is generally performed at special healthcare facilities, resulting in limited accessibility to patients, specifically in rural areas. PSG is expensive and patients have limited access to this specialized testing. In recent years, the use of less expensive, more accessible portable home monitoring to diagnose and manage patients with OSA has gained favor, but studies regarding its use and patient outcomes are lacking.
The report summarizes the proceedings and recommendations of an international workshop sponsored by the American Thoracic Society (ATS), the American Academy of Sleep Medicine (AASM), the American College of Chest Physicians (ACCP) and the European Respiratory Society (ERS) that convened to determine research priorities that can help incorporate portable monitors safely into healthcare practices.
"The consensus of the workshop participants was that outcomes-based research studies are needed to demonstrate the efficacy and cost effectiveness of portable monitor testing," said Samuel Kuna, MD, associate professor of medicine at the University of Pennsylvania and chief of the Pulmonary, Critical Care & Sleep Section at Philadelphia Veterans Affairs Medical Center, and chair of the workshop's steering committee. "There is also a need to develop clinical sleep research networks capable of performing large, prospective studies."
Recommendations were developed regarding research study design and methodology, including the need to standardize technology, identify patients who would be "best fit" for ambulatory management of OSA, ensure patient safety and identify sources of research funding.
"While attempting to validate portable monitors, we need to understand the significant clinical limitations of PSG and work to further standardize the sensors, signal processing and protocols used in this 'gold-standard' test," Dr. Kuna said. "Similar efforts are needed to further standardize portable monitors, especially to allow study results to be compared across monitors."
In addition, Dr. Kuna said more clinical trials are needed to compare the treatment outcomes of both home and in-laboratory testing for different types of patients, and to determine cost-effectiveness.
"Current portable-monitor technology seems to be most applicable in populations having a high likelihood of OSA," he noted. "Ideally, alternative approaches should also be made available to underserved and remote populations that do not have access to gold-standard testing."
"Studies that include cost-effectiveness as an outcome will allow decision-makers to develop healthcare policies regarding the clinical application of portable monitor testing for the ambulatory management of patients with OSA," he said.
"Pressure for alternative approaches to current recommended in-laboratory management of patients with OSA will continue to increase given the cost of PSG and the limited number of laboratory facilities relative to patient need," Dr. Kuna continued. "Clinical demand for more rapid access to testing will also likely increase as more studies link treatment of OSA to improved cardiovascular outcomes for patients."
The need for ambulatory testing and management options will also likely increase as the field of sleep medicine evolves and expands, Dr. Kuna said.
"As physicians in family practice and otolaryngology join pulmonologists, psychiatrists, and neurologists to specialize in sleep medicine, the desire to test populations outside of the sleep center will grow," he said. "High-quality research will be needed to guide the systematic development of these alternative clinical disease management pathways."