New breast cancer model of mutant PI3K recapitulates features of human breast cancer
Scientists from the Friedrich Miescher Institute for Biomedical Research have shown that a mutation in the lipid kinase PI3K, which occurs in about 30% of human breast cancers, itself evokes different forms of breast cancer. While this kinase has long been associated with cancer, and is a target for anti-tumor therapy, it is now shown to be causal for multiple types of breast cancer.
Almost every sixth cancer diagnosis in women is breast cancer. Although various treatments exist for different kinds of breast cancers and although the 5-year survival rate has reached 85%, breast cancer is still the second-most common cause of cancer death after lung cancer. It is therefore vitally important to identify the molecular and cellular alterations that cause the disease.
Mohamed Bentires-Alj, his PhD student Dominique Meyer and collaborators have now published a study that addresses the role of the phosphoinositide 3-kinase (PI3K) signaling pathway in the development of breast cancer. Several proteins in this signaling cascade are known to play a role in this disease. In particular, mutations in the catalytic subunit of PI3K itself, encoded by a gene called PIK3CA, occur in approximately 30% of human breast cancers. However, it was not clear if these mutations alone can initiate the disease and what their contribution was during the development of the disease state.
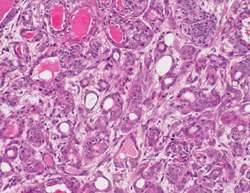
These FMI scientists now show that the H1047R mutant form of PIK3CA is sufficient to cause tumors in the mammary tissue of mice. "Importantly, the mutation caused a variety of breast cancer histotypes," comments Bentires-Alj. "This indicates that the mutation has its strongest effect in precursor cells that give rise to several different cell types. Thus, our model recapitulates features of human breast tumors with the same mutation. It will be used for testing PI3K inhibitors, some of which are already in clinical trials. This type of model will allow us to predict potential resistance mechanisms to this targeted therapy." Indeed, by identifying pathways of resistance, optimal combination therapies for cancer can be designed to improve existing and future therapies.
More information: Meyer DS, et al. (2011) Luminal expression of PIK3CA mutant H1047R in the mammary gland induces heterogeneous tumors. Cancer Res 71:4344-5













