Technique to stimulate heart cells may lead to light-controlled pacemakers
(Medical Xpress) -- A new technique that stimulates heart muscle cells with low-energy light raises the possibility of a future light-controlled pacemaker, researchers reported in Circulation: Arrhythmia & Electrophysiology, a journal of the American Heart Association.
"Electronic cardiac pacemakers and defibrillators are well established and successful technologies, but they are not without problems, including the breakage of metal leads, limited battery life and interference from strong magnetic fields," said Emilia Entcheva, Ph.D., senior author of the study and associate professor of biomedical engineering at Stony Brook University in Stony Brook, New York. "Eventually, optical stimulation may overcome some of these problems and offer a new way of controlling heart function."
The research is part of a new field called optogenetics that introduces light-sensitive proteins into "excitable" cells, making it possible to control specific activities within cells. Excitable cells can actively generate electrical signals such as nerve cells and muscle cells.
The main appeal of control by light is the unprecedented ability to remotely, without contact, turn on/off a single cell or a cell type, not possible by electrical or other means of stimulation.
Several years ago, investigators discovered that brain cells could be stimulated using light if they were genetically altered to produce a light-sensitive protein called channelrhodopsin 2 (ChR2).
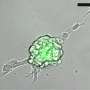
In the new study, researchers created cells expressing the ChR2 protein and coupled them with heart muscle cells from animals, creating heart tissue stimulated by light. They found light-triggered heart muscle contractions and electrical waves were indistinguishable from electrically-triggered waves.
Rather than directly modifying heart cells, the researchers coupled donor cells optimized for light responsiveness with the heart cells. The new technique uses much lower energy than in prior studies and doesn't require the use of viruses or the introduction of genes from other organisms into heart cells. Instead, cells from a person's bone marrow or skin can be cultured and modified to respond to light, reducing the possibility that the immune system will reject the light-sensitive cells.
"Our method of non-viral cell delivery may overcome some hurdles toward potential clinical use by harvesting cells from the patient, making them light-responsive and using them as donor cells in the same patient," Entcheva said.
The approach may someday improve pacemakers and defibrillators. Instead of metal leads, a light-controlled pacemaker would use biocompatible, flexible plastic optic fibers.
In preliminary calculations, a light-based system might require only one-tenth the energy, meaning that a battery could last 50 years rather than five. The more immediate application of the technique will likely be to aid heart research.
"Optical stimulation is a great tool to selectively probe and control different parts of the electrical circuitry of the heart to better understand where the vulnerable sites are or what gives rise to lethal arrhythmias," Entcheva said.
The technique might also be used to test new drugs for possible cardiac side effects.