Eye research paves way for more successful cornea transplants
(Medical Xpress) -- Scientists at the University of Reading have made a significant breakthrough in cornea transplant research that could make future procedures more successful.
Amniotic membrane (AM) has been used in the clinical treatment of eye disorders for over a decade. During this time it has been seen as an excellent natural surface on which to grow corneal stem cells, despite the fact that its structural and biological properties have been poorly understood.
Furthermore, regardless of AM's many reported successful ophthalmic outcomes, the resulting clinical efficacy has lacked predictability - its success rate, when used in conjunction with stem cells, ranges from 46% to 100%.
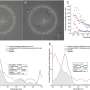
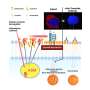
Researchers from Reading have now shown that the location of the AM, relative to the placenta, plays a crucial part in its success as a biomaterial. AM taken nearer to the placenta is stiffer than that taken from further away, and this difference in mechanical properties dramatically effects the functionality of the stem cells. This is particularly pertinent as the underlying clinical reason for using AM is that the transplanted cells should remain in a relatively unchanged state to maximize their clinical effect.
Dr Che Connon, from Reading School of Pharmacy, said: "Our work suggests that clinical results could be improved by using AM collected from an area close to the placenta, or by normalizing the substrate's mechanical properties (stiffness), chemically, prior to use.
"Until now no consideration has been given to the origin of the AM, relative to the placenta, when used as a surface for the expansion of stem cells prior to transplantation. Our new research should improve the success of the procedure."
More information: The paper, The mechanical properties of amniotic membrane influence its effect as a biomaterial for ocular surface repair, by Bo Chen, Roanne R. Jones, Shengli Mi, James Foster, Simon G. Alcock, Ian W. Hamley and Che J. Connon, appears in Soft Matter, DOI:10.1039/C2SM26175H