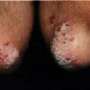
Study examines risk of heart attack associated with various psoriasis treatments
Use of tumor necrosis factor (TNF) inhibitors for treatment of psoriasis is associated with a significantly reduced risk for heart attack (myocardial infarction) compared to other forms of treatment, according to a report published Online First by Archives of Dermatology.
"The effect of systemic treatment for psoriasis on cardiovascular disease has been largely unexplored," the authors write as background information in the study. "The primary objective of this study was to assess whether patients with psoriasis treated with TNF inhibitors have a decreased risk of MI [myocardial infarction] compared with those not treated with TNF inhibitors (i.e., those who received oral agents/phototherapy or topical agents)."
Jashin J. Wu, M.D., of the Kaiser Permanente Los Angeles Medical Center, and colleagues, conducted a retrospective study that included patients with at least three ICD-9-CM codes for psoriasis or psoriatic arthritis, without antecedent MI, between January 2004 and November 2010.
Of the 8,845 patients included in the study, 5,075 (57.4 percent) were not treated with any systemic therapy or phototherapy (topical treatment group), 1,673 (18.9 percent) received a TNF inhibitor for at least two consecutive months (TNF treatment group) and 2,097 (23.7 percent) were treated with oral systemic agents or phototherapy (oral/phototherapy treatment group).
After adjusting for other MI risk factors, patients in TNF inhibitor treatment group and the oral/phototherapy treatment group had a significantly lower risk of MI (50 percent and 46 percent, respectively) compared with patients in the topical treatment group. Differences in risk between the TNF inhibitor group and oral/phototherapy group did not reach statistical significance.
"Future prospective studies are needed and warranted to determine whether the use of TNF inhibitors may reduce the risk of major adverse cardiovascular events in patients with systemic inflammatory conditions," the authors conclude.
More information: Arch Dermatol. Published online August 20, 2012. doi:10.1001/archdermatol.2012.2502