Study to examine methods to reduce damage of radiotherapy to normal tissue
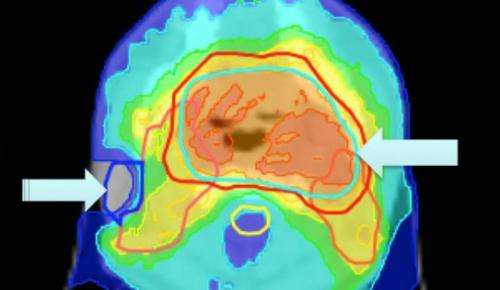
About half of all people with cancer receive a course of radiotherapy, a form of treatment in which X-rays are used to shrink or destroy the tumour. With the benefit of advanced systems, it is now possible to aim radiation beams at tumours more effectively than ever before, allowing increasing doses of radiotherapy with increased cancer cure rates, and also reducing side effects.
However, although clinicians use planning software to define the target area for treatment and deliver the optimal dose, any dose that falls outside the target area – for instance due to the positioning of the patient and their internal organs during treatment – can cause permanent and severe damage to normal tissues.
Now, a new research programme at the University of Cambridge aims to reduce levels of toxicity from radiotherapy, enabling doses of the treatment to be escalated. By examining to what extent the dose of radiation planned by the clinician for a patient differs from that which the patient actually receives – and how this damages normal, healthy tissues – the programme will develop a set of tools that can be used to provide patients with the optimal dosage for their condition.
"We are breaking new ground thanks to the marshalling of forces from several fields," said Professor Neil Burnet, who leads the research. Expertise is being pooled from a cross-disciplinary group of clinicians and scientists from the University of Cambridge Departments of Oncology, Physics, Engineering, and Applied Mathematics and Theoretical Physics, the NHS Oncology Centre, and the Cancer Research UK (CRUK) Cambridge Research Institute.
"The aim will always be to safely deliver radiation to the tumour and so kill the cancerous cells," he added. "Although modern technology has improved side effects, 29% of patients are still left with significant dry mouth after head and neck radiotherapy because of damage to the salivary glands, and 10% of men experience severe toxicity after prostate radiotherapy because of rectal damage. Hormonal dysfunction after radiotherapy damage to the hypothalamus and pituitary gland can result in a patient needing lifelong hormone replacement therapy."
The VoxTox Research Programme, a five-year study funded by CRUK, focuses on reducing radiation toxicity. After quantifying the differences between planned dose and the dose actually delivered during the whole course of radiotherapy, the programme will link these data to differences between expected and observed toxicity. It will look into the physical factors behind dose variation such as movement of internal organs, as well as suspected biological factors, such as a patient's genetic make-up.
"In Cambridge there is a unique archive of daily computed tomography (CT) scans – imaging data acquired during the course of a patient's high-precision image-guided radiotherapy on our TomoTherapy treatment machines," said Burnet. "Systems will be developed to map the location of each point, or voxel, within the patient outline, and then to re-compute the dose at that point each day during treatment."
The study will develop a suite of integrated software tools for dose review during the treatment course, with the objective of individualising treatment based on predicted toxicity, and make these tools available to the world cancer community.