Exercise rate related to improvements in Parkinson's disease
People with Parkinson's disease benefit from exercise programs on stationary bicycles, with the greatest effect for those who pedal faster, according to a study presented today at the annual meeting of the Radiological Society of North America (RSNA). Functional connectivity magnetic resonance imaging (fcMRI) data showed that faster pedaling led to greater connectivity in brain areas associated with motor ability.
Parkinson's disease is a chronic, progressive disorder of the central nervous system. Early-stage symptoms like shaking and difficulty with walking eventually may progress to cognitive and behavioral problems such as dementia. An estimated 7 to 10 million people worldwide live with Parkinson's disease, according to the Parkinson's Disease Foundation, with most cases occurring after the age of 50.
As the disease progresses and the frequency of side effects increases, the therapeutic window begins to close. Deep brain stimulation is an effective therapy for late-stage Parkinson's disease, but is an invasive and costly procedure.
Exercise is thought to have beneficial effects on Parkinson's disease. Jay L. Alberts, Ph.D., neuroscientist at the Cleveland Clinic Lerner Research Institute in Cleveland, saw this firsthand in 2003 when he rode a tandem bicycle across Iowa with a Parkinson's disease patient to raise awareness of the disease. The patient experienced improvements in her symptoms after the ride.
"The finding was serendipitous," Dr. Alberts recalled. "I was pedaling faster than her, which forced her to pedal faster. She had improvements in her upper extremity function, so we started to look at the possible mechanism behind this improved function."
As part of this inquiry, Dr. Alberts, researcher Chintan Shah, B.S., and their Cleveland Clinic colleagues, recently used fcMRI to study the effect of exercise on 26 Parkinson's disease patients.
"By measuring changes in blood oxygenation levels in the brain, fcMRI allows us to look at the functional connectivity between different brain regions," Shah said.
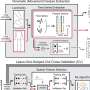
The patients underwent bicycle exercise sessions three times a week for eight weeks. Some patients exercised at a voluntary level and others underwent forced-rate exercise, pedaling at a speed above their voluntary rate. The researchers used a modified exercise bike to induce forced-rate activity.
"We developed an algorithm to control a motor on the bike and used a controller to sense the patient's rate of exertion and adjust the motor based on their input," Dr. Alberts said.
fcMRI was conducted before and after the eight weeks of exercise therapy and again as follow-up four weeks later. The research team calculated brain activation and connectivity levels from the fcMRI results and correlated the data with average pedaling rate. Results showed increases in task-related connectivity between the primary motor cortex and the posterior region of the brain's thalamus. Faster pedaling rate was the key factor related to these improvements, which were still evident at follow-up.
"The results show that forced-rate bicycle exercise is an effective, low-cost therapy for Parkinson's disease," Shah said.
Dr. Alberts noted that that while faster pedaling led to more significant results, not all Parkinson's patients need to do forced-rate exercise to see improvement.
"We're now looking at this phenomenon in patients with exercise bikes in their home," he said, "and other exercises like swimming and rowing on tandem machines may provide similar benefits."