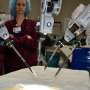
Johns Hopkins surgeons among the first in the country to perform a robotic single-site hysterectomy
Two Johns Hopkins gynecologic surgeons are among the first in the nation to perform a robotic hysterectomy using a single, small incision.
Amanda Nickles Fader, M.D., associate professor of gynecologic oncology and director of the Kelly Gynecologic Oncology Service and the Minimally Invasive Surgery Center in the Department of Gynecology and Obstetrics; and Stacey Scheib, M.D., assistant professor of gynecology and obstetrics and director of the Multidisciplinary Fibroid Center in the Division of Gynecologic Specialties at Johns Hopkins, recently performed other several types of single-site robotic gynecologic procedures—including surgery for fibroids, abnormal uterine bleeding and ovarian cysts and masses.
Nickles Fader and Scheib have collectively authored more than 25 articles on robotic surgery as well as single-site laparoscopy in peer-reviewed medical journals. They are among a small group of surgeons in the United States, with expertise in this procedure, according to officials at The Johns Hopkins Hospital.
Nickles Fader, an internationally recognized surgeon with a specialty in minimally invasive women's cancer surgery, has performed more than 400 laparoscopic single-site surgeries and more than 600 robot-assisted procedures since 2008.
"To be one of the first hospitals in the region to offer this surgical innovation, which is a less invasive surgical option for many women, demonstrates Johns Hopkins' commitment to providing our patients with the most advanced, minimally invasive surgical options," says Nickles Fader. "Our institution is also leading the way with surgical innovations research, to ensure that any new technology we use in the operating room is safe, cost-effective and truly better for our patients than what we have used in the past."
Scheib, a nationally known expert in the single-incision laparoscopic technique for hysterectomies and other gynecologic procedures, who has performed more than 600 single-site procedures since 2009, says, "I think this is only the beginning and eventually we will expand the use of this tool for more procedures."
Recently approved by the U.S. Food and Drug Administration, single-site robotic surgery offers the traditional benefits of minimally invasive surgery such as shorter recovery time, smaller incisions, minimal pain, low blood loss and a brief hospital stay, but it also provides the added benefit of a single incision, so that women are left with just one, nearly invisible scar.
Conventional laparoscopy and robotic surgery both offer the promise of less invasive surgery to treat both benign and cancerous gynecologic conditions. These approaches, in which several small surgical incisions are made in the abdomen instead of one large incision, lead to faster recovery times, less pain and a better experience for women who need a hysterectomy or other gynecologic procedure.
Single-site surgery goes even farther, allowing surgeons to perform complex abdominal procedures through a single, tiny incision in the belly button. Benefits of this approach include the cosmetically hidden surgical scar at the base of the navel. Additionally, the navel is the thinnest part of the abdominal wall, with few nerves, blood vessels and little muscle, so patients may avoid incisions through their abdominal muscles and may experience less pain after the surgery. During a robotic-assisted single-site procedure, the surgeon sits at the robotic console, viewing a 3-D, high-definition camera image of the surgical site. The surgeon uses hand controls to move the camera and instruments—controls that translate hand, wrist and finger movements into more precise movements of the smaller instruments inside the patient.