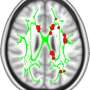
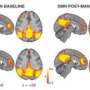
UCLA to house worldwide database of brain images for chronic-pain conditions
What do migraine, irritable bowel syndrome, fibromyalgia and rheumatoid arthritis have in common? All involve chronic pain.
A new database featuring hundreds of brain scans and other key clinical information will help researchers tease out similarities and differences between these and many other chronic-pain conditions, helping to accelerate research and treatment development.
The Gail and Gerald Oppenheimer Family Center for Neurobiology of Stress at UCLA will serves as the main hub for this new Pain and Interoception Imaging Network (PAIN), the first-ever standardized database for brain imaging associated with chronic pain. So far, 14 institutions in North America and Europe are participating.
Building upon their experiences creating a similar but smaller network to study pelvic pain, the UCLA team is now developing this larger chronic-pain network with the help of a $300,000 grant from the National Institutes of Health.
"We are now recognizing that chronic pain is a brain disease, and if we want to treat it more effectively, we need to better understand and treat the mechanisms in the brain that are driving it," said Dr. Emeran Mayer, a professor of medicine in the divisions of digestive diseases, physiology and psychiatry at the David Geffen School of Medicine at UCLA and executive director of the Gail and Gerald Oppenheimer Family Center for Neurobiology of Stress at UCLA.
According to Mayer, brain imaging is one of the most promising technologies for breakthrough findings in chronic pain. However, research is currently significantly limited, due to the fact that most institutions can only support small studies on their own and lack access to large samples of patients. In addition, there is no standardization of acquired data, making it difficult to combine brain scans from multiple investigators that are obtained using different scanners, techniques and sets of clinical data.
That will change with the new PAIN. The aim is for the network to include information from more than a thousand patients, including both adults and children.
In addition to brain scans, researchers will also have access to clinical and biological information on patients—the so-called "metadata"—including symptom measures; psychosocial factors; gene expression; immune system information; data on bacteria in the intestines, known as gut microbiota; and environmental data. Researchers can then develop large, overlapping data sets to pinpoint similarities and differences among chronic-pain conditions and correlate brain scans with clinical metadata.
"Like a fingerprint, researchers will be able to pick out distinct patterns from the scans of individuals with each pain condition and, combined with additional information provided by the network, assess how chronic pain manifests differently between men and women, across the life span, or between conditions," said Dr. Bruce Naliboff, a professor in the departments of medicine and psychiatry and biobehavioral sciences at the Geffen School of Medicine and co-director of the Gail and Gerald Oppenheimer Family Center for Neurobiology of Stress.
Dr. Kirsten Tillisch, a UCLA associate professor of digestive diseases who directs the neuroimaging core at the Oppenheimer Center, points out that in the future, PAIN will also include information about the tens of trillions of microbes that make up the bacteria living in the intestines. She notes that each patient's gut microbiota is unique, like a signature card.
"Researchers are now exploring the connection between the brain and gut, and the type of bacteria living in the intestine may also play a role in some forms of chronic visceral pain," said Tillisch.
The standardized brain scans will include structural data on grey and white matter and on intrinsic oscillations of the brain—"resting state scans." Such scans are obtained when the brain is not engaged in a particular task.
Mayer adds that PAIN may also help researchers in the future identify and pinpoint appropriate treatments by targeting subsets of conditions.
"The more information we can gather about each individual chronic-pain condition, the better we'll be at predicting how subsets of patients will react to therapies," he said.