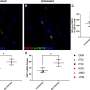
Experimental HIV vaccine targets virus envelope protein
AIDS research has investigated many strategies to tackle the HIV virus. Now, a new type of vaccine developed within the EU-funded project EuroNeut-41, targets an HIV envelope protein called the gp41. The protein is directly responsible for the fusion of the HIV virus with human cells. By integrating the gp41 protein into the vaccine, researchers are attempting to trigger the production of antibodies that would block the entrance of HIV into human cells.
"We have used an innovative approach, combining protein engineering, specific vaccine formulation, and a combination of routes of administration, [nasal] and intramuscular," says Nicolas Mouz, chief scientific officer at PX'Therapeutics, one of the project partners. The company is also providing protein engineering research and manufacturing. It is located in Grenoble, France.
There have been many vaccine trials since the discovery of the virus in the early 1980s, seeking both a cure for infected people and a preventative therapy to stop the contagion. "This gp41 protein from the virus envelope is not an absolute novelty in the long history of anti HIV vaccine development," says Alexandru Rafila, Chairman of the Romanian Society for Microbiology in Bucharest. "But it is a meaningful approach in protein design that could be given as a vaccine so that it triggers an immune response."
The trouble is that the virus targets not only the lymphocyte cells, which include T cells—a key component of the body's immune system helping to fight diseases—but also other immune system cells. The latter are not exclusively infected through the gp41 protein but also through other mechanisms. "An efficient vaccine should hamper the infection of any other cells," Rafila says.
Other experts concur that the diversity of HIV and its enormous capacity to mutate are major challenges for vaccine development. "The idea basically is that a vaccine should induce antibodies T cells immune response, that would neutralise HIV in all of its forms," says Ulrich Fruth, vaccine development and evaluation team leader at the World Health Organisation, in Geneva, Switzerland.
Even though Fruth considers the project strategy a viable approach, chances of success for this vaccine are difficult to predict. "We just don't know," he says. "The only thing we know is that we have more experience on human trials. The animal models used so far were not very predictive. We need human clinical trials in order to decide which vaccine to take forward." The vaccine is in its first stage of clinical safety studies, which demonstrated a relatively weak effect. It is still too early to draw conclusions.
In addition, Fruth points to a minor limitation of this vaccine, namely that it focuses on the induction of antibodies. He says, "We think that for a successful protection we may need [to target] both: antibodies and T cells. The role that I would see for such a vaccine would probably be in combination with the components that induce T cell immune response. So, [what may prove useful is to test] a combination vaccine [and] not a standalone one."