MRI-guided procedure tested as non-invasive study procedure for uterine fibroids

On April 11, 2013, Kimberly Dull became the first woman in Illinois—and one of the first in the United States—to take part in a clinical trial of an investigational, non-invasive procedure for uterine fibroids. The procedure, known as MRI-guided HIFU, uses magnetic-resonance imaging to focus heat-generating, high-intensity ultrasound onto these growths.
Researchers are testing whether MRI-guided HIFU could lead to quicker recovery with fewer after-effects than current treatments, such as surgical removal of the uterus. The HIFU procedure does not require an incision or general anesthesia. Subjects are typically discharged from the hospital that day.
Because this is a controlled clinical trial, four out of five volunteers will receive the study procedure. One out of five will go through the full protocol but will not receive HIFU, and thus not experience any study procedure-related change in her fibroids. Subjects will not be told whether they were given the study procedure or not until the three-year study is completed.
"It all went smoothly," Dull reported. "I went home the same day and felt completely normal."
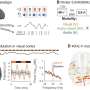
The trial brings together two rapidly advancing technologies: high-resolution magnetic resonance imaging (MRI) and high-intensity focused ultrasound (HIFU). The MRI guides and monitors therapy. HIFU's concentrated sound waves generate heat, which can destroy fibroids. This approach is designed to have little or no effect on the healthy tissues around fibroids.
"MRI-guided HIFU has the potential to treat uterine fibroids in a non-invasive way," said trial director Aytekin Oto, MD, professor of radiology and surgery and director of abdominal magnetic resonance imaging at the University of Chicago Medicine. "Subjects are not exposed to surgery or radiation and should be able to return to daily normal activities the day after undergoing this procedure."
The University of Chicago Medicine is seeking about 30 participants for this study. Volunteers must be less than 50 years old, have fibroids that affect their quality of life, and have no intention of getting pregnant.
The medical center is one of only five sites for this study in the United States. There are four additional sites in Canada and Korea.
Uterine fibroids are extremely common, occurring in 20 to 50 percent of women older than 30 years of age. These benign tumors grow in the muscle layers of the uterus, where they can cause cramping, pain, heavy menstrual bleeding, constipation, bloating and frequent urination.
Hysterectomy (surgical removal of the uterus) is the most common treatment, requiring anesthesia, a hospital stay and recovery at home. Many women choose less-invasive approaches to symptomatic relief, such as myomectomy (surgical removal of just the fibroids) or uterine artery embolization (which blocks blood flow to the affected tissue).
"MRI-guided HIFU may turn out to be the next step in this shift toward less and less invasive therapies," said co-investigator in the trial, Nathaniel Crump, MD, assistant professor of obstetrics and gynecology at the University of Chicago Medicine.
The procedure requires the subject to lay face-down on a special MRI table with a flexible gel pad wrapped around her abdomen. Real-time MRI scans guide the ultrasound procedure and monitor temperatures in and around targeted tissues.
During the procedure, which can last a few hours, subjects have a urinary catheter inserted to drain the bladder. Subjects may also have an intravenous line inserted, as needed, for pain relief or conscious sedation. Once the ultrasound is finished, subjects receive an injection of a contrast agent that enhances MRI assessment of the effects.
"The worst part was lying still so long," said Jennifer Smith, the second subject enrolled in the study. "I felt some discomfort, but I walked out of the hospital 30 minutes after it was over and went out to lunch. The next day I went downtown shopping. I'm hopeful that this will make a difference and I'm telling lots of people about the trial."
Subjects must come back for five scheduled follow-up visits over the next three years.
Women enrolled in the trial will not be charged. They will be compensated for the inconvenience of participation, including the required collection of menstrual-flow samples before and after the study procedures.