February 13, 2014 feature
When less is more: Microglia deficit impairs functional neural connectivity, leads to autism-associated behaviors
(Medical Xpress)—Extensive research effort has been focused on determining the genetic and cellular factors leading to neurodevelopmental illnesses such autism, Asperger's syndrome and schizophrenia. Oftentimes, however, while a given factor – for example, a microdeletion (the loss of a chromosomal fragment) or a particular cell type such as microglia (which infiltrate the developing brain and help prune synapses during brain maturation) – is associate with neurodevelopmental illnesses, the actual phenotypical mechanism remains unknown. Recently, however scientists at the European Molecular Biology Laboratory (EMBL) in Monterotondo, Italy made the genotype-phenotype connection, demonstrating that laboratory mice in which the Cx3cr1 gene is removed, or knocked out (KO) – referred to as Cx3cr1KO mice – exhibit a microglia deficit during development that, in turn, causes reduced functional brain connectivity and autism-linked behaviors that persist into adulthood.
EMBL Senior Scientist Dr. Cornelius Gross discussed the paper that he, Dr. Yang Zhan and their co-authors published in Nature Neuroscience, demonstrating that a deficit in microglia was sufficient (rather than correlated with or a secondary consequence of) to cause autism-related behavioral and functional connectivity deficits in mice. "By using mice that lack the Cx3cr1 gene that's expressed only in microglia in the brain," Gross tells Medical Xpress, "we were very sure to have only altered microglia, and that a deficit in microglia were responsible for the changes in connectivity and behaviors we saw. We're therefore quite certain that the changes we see in connectivity and behavior are due to a problem with microglia," Gross tells Medical Xpress, "because that's the only place in the brain where the Cx3cr1 gene we removed is expressed." He adds that the gene is also expressed in some immune cells in other parts of the body, so theoretically those could also be responsible – but that he thinks this unlikely.
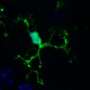
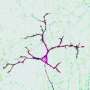
Understanding exactly how microglia promote the maturation of circuit connectivity during development is another matter. "During the period of development when synapses – the connections between neurons – are formed, neurons begin to talk to microglia," says Gross. "In our mice, we've broken that conversation. As a result, microglia are no longer able to efficiently carry out their program of eliminating, or pruning, synapses." The researchers went on to show that with less synaptic elimination, the remaining synapses are unable to strengthen properly, and so develop a feature of brain circuits called synaptic multiplicity.
The paper also reports that the scientists established the neurodevelopmental role that microglia play in circuit connectivity maturation. "The ligand for Cx3cr1 is a chemokine, called fractalkine (Cx3cl1), that is expressed by neurons in the brain," Gross points out. (In this case, the ligand is a protein that binds to Cx3cr1, which is a protein and cell surface receptor, while chemokines are a family of small cytokines, or signaling proteins secreted by cells.) "We engaged in this research because we identified fractalkine as a gene that gets expressed for the first time in neurons that are making their connections – and not earlier." Given that the receptor was only on microglia, the scientists hypothesized that neurons need to talk to microglia during this period of synapse formation to do something – and because microglia are phagocytic cells, they thought it likely that this function was synapse elimination. (Phagocytic cells protect the body by ingesting harmful particles, bacteria, and dead or dying cells in a process called phagocytosis.)
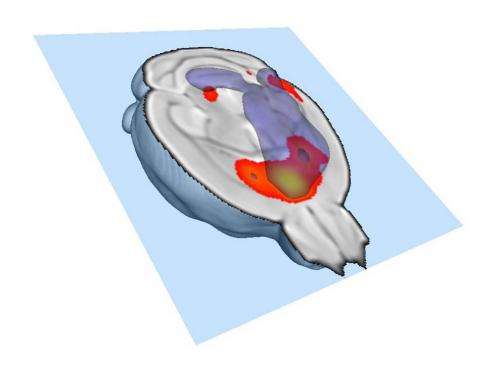
"Initially a neuron makes a single connection on a target neuron, and the synaptic multiplicity, or number of contacts between neuron pairs, is one," says Gross, "but later additional connections are made and synaptic multiplicity increases – and higher synaptic multiplicity means more effective signaling between neurons. That said, our data suggest that in order to make some connections stringer you have to eliminate others. Moreover, the fact that neurons in these microglia-deficient mice never increased their synaptic multiplicity told us that they have weak functional connections." Gross and his colleagues then collaborated with physicists at the Italian Institute of Technology to carry out functional magnetic resonance imaging on their mice to determine if their brains were well-connected. "We were quite shocked to see that the different regions of the brain were just doing their own thing – essentially ignoring each other," relates Gross. "Moreover, the connectivity pattern resembled what we see in autism using the same technology, with major deficits seen in connections with the prefrontal cortex." The researchers are now studying how this actually occurs.
One of the team's key insights was that low synaptic multiplicity might lead to weak functional connectivity at the level of gross brain structures. "I got this idea from reading the autism clinical literature in which weak functional connectivity has been widely studied, but where no one had yet been able to propose a mechanism," Gross points out. "Another key insight we took from the autism literature was a control trial we performed in our social behavior experiments. Since we used mothers as social partners, we tested a mother immobilized through anesthesia in our social interaction tests, and they no longer had a deficit – something no one has done before in mouse models of autism. We found that social behavior in our mice was fine if the social partner was not moving suggesting that it was something about the reciprocal nature of the social behavior that they were avoiding. Some people have argued that the antisocial behavior of autistic individuals derives from a problem in evaluating the intention of others – so there could be a parallel there with our mice.
The paper states that the study's data open the possibility that genetic and environmental risk factors for neurodevelopmental disorders like autism may exert their effect by modulating synapse elimination – and therefore that further studies are warranted to test the hypothesis that variation in synaptic pruning may underlie individual differences in human brain wiring and behavior. "The idea is not that people get autism by having a mutation in Cx3cr1 – although this has not yet been formally tested – but that low synaptic multiplicity might be the culprit in at least some cases of autism," says Gross. "This low synaptic multiplicity could be due to a deficit in microglia as in our mice, but it could also be due to problems in other aspects of synapse formation. Most of the well documented genetic cases of autism, for example, seem to involve synaptic proteins. On the other hand, microglia are exquisitely sensitive to infection and maternal infection during gestation could have long term effects on their function." In other words, synaptic multiplicity might be a common mechanism for a poorly-connected brain, and this might occur through genetic and/or environmental means. Gross notes also that other neurodevelopmental disorders, including schizophrenia, epilepsy and major depression, often show weak functional connectivity – so this model may be relevant for these disorders as well.
Do the paper's findings suggest the possibility of translational or regenerative therapies for ameliorating or reversing neurodevelopmental reduced functional connectivity? "This is more difficult," Gross says. "There are people who are thinking that blocking or promoting microglia phagocytosis might be therapeutic, but this seems to happen in humans just before birth or shortly after – and it's not clear that the deficits can be reversed later. I think a more promising approach would be to use neuromodulators to make neuronal contacts with low synaptic multiplicity act like ones with high synaptic multiplicity by boosting glutamatergic neurotransmission." Neuromodulators are substances other than neurotransmitters that can increase or decrease the effect of neurotransmitters.
Moving forward, says Gross, the scientists are trying to catch microglia in the act of ingesting synapses, as well as figuring out why some synapses get eaten and other not – does this happen on a random basis, for example, or because they are less active, or have been misassembled. Further afield, Gross notes that other areas of research might benefit from their study. "Our resting state fMRI data is innovative, and in fact has never been done in transgenic mice. Moreover," Gross concludes, "our validation of resting state fMRI, or rs-fMRI," – a method of functional brain imaging that can be used to evaluate regional interactions that occur when a subject is not performing an explicit task – "using EEG coherence electrophysiology is very interesting to the researchers in the fMRI field, since there's been much criticism about what the fMRI signal really reflects."
More information: Deficient neuron-microglia signaling results in impaired functional brain connectivity and social behavior, Nature Neuroscience published online 02 February 2014, DOI: 10.1038/nn.3641
© 2014 Medical Xpress. All rights reserved.