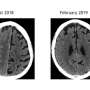
Two spine surgeons are three times safer than one

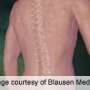
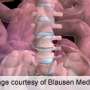
A new team approach has improved safety—reducing rates of major complications by two thirds—for complex spinal reconstructive surgery for spinal deformity in adult Group Health patients at Virginia Mason Hospital & Seattle Medical Center.
An article in the March issue of Spine Deformity gives a detailed description of the standardized protocol before, during, and after the surgery, stressing the new approach's three main features:
- Two spine surgeons in the operating room
- A live preoperative screening conference
- Monitoring bleeding during the operation
The research team reviewed 164 consecutive patients: 40 before and 124 after the new three-pronged approach was implemented. After implementation, patients were three times less likely to develop major complications. Improvements included significant reductions in rates of wound infection, deep vein thrombosis, pulmonary embolism, and urinary tract infections. Patients were also significantly less likely to have to return to the operating room within 90 days after the surgery.
"We can shorten the operation when we have two surgeons in the operating room as equal partners: a neurosurgeon and an orthopedic surgeon with specialized spine training," said lead author Rajiv K. Sethi, MD. He is an orthopedic spinal surgeon in the neurosurgery department at Group Health Physicians, the director of spinal deformity and complex reconstruction at Virginia Mason, and a clinical assistant professor of health services at the University of Washington (UW) School of Public Health.
"Reconstructive surgery for adults with spine deformities like scoliosis and kyphosis is being done increasingly often," Dr. Sethi said. "But this kind of surgery tends to be long and difficult, and it is among the most dangerous and complication-ridden of all operations. And often the outcomes and complications are unacceptable, including some patients losing more blood than they started with." That's why the new approach uses a standardized protocol to monitor and manage any bleeding during the operation.
The new approach also involves a feature that has never been described before: a live conference with clinicians from various disciplines. They are the operative surgeons, an internist, a physical medicine and rehabilitation physician, the nurses who coordinate a class for complex spine patients, and at least two members of the anesthesiology team dedicated to complex spine surgery. Together, they identify and treat health and medication issues that, undetected, might otherwise have derailed an operation at the last minute. Planning well in advance, they discuss—and decide—whether proposed surgery is appropriate for each patient.
"Our findings could help medical teams at Group Health and around the country reduce complications—and likely cut costs too—while improving performance and patient outcomes," Dr. Sethi said. "But all clinicians at Group Health and Virginia Mason are paid on salary. By contrast, at medical centers where doctors are paid on a fee-for-service basis, with more pay for doing more procedures, it might be harder to institute this kind of systems approach, because it entails up-front costs and commitment from leadership."